Wound dehiscence can occur after surgery when a previously closed incision partially or completely reopens. This separation exposes the underlying tissues and significantly increases the risk of infection and other complications.
While it most commonly occurs between five and eight days after surgery, it can develop at any point before full healing is achieved.
Both external incisions and internal surgical wounds can be affected. When the wound edges separate, the body becomes more vulnerable to infection, delayed healing, and additional complications that may require further medical intervention.
Because it can interfere with the body’s natural healing process, wound dehiscence requires timely evaluation and appropriate care.
What is wound dehiscence?
Wound dehiscence is a complication in which a surgical incision partially or completely reopens after it has been closed. It most often develops between five and eight days after surgery, although it can happen at any time before healing is complete. This separation exposes underlying tissues and increases the risk of infection and delayed recovery.
What are the common signs and symptoms of wound dehiscence?
Visible separation of the wound is the most obvious sign, ranging from a small opening to a complete reopening. Patients may also experience increased pain, swelling, drainage of blood or pus, and sometimes an unpleasant odor. These symptoms indicate that medical evaluation, be it at a wound care center or in a location of your choosing, is necessary as soon as possible.
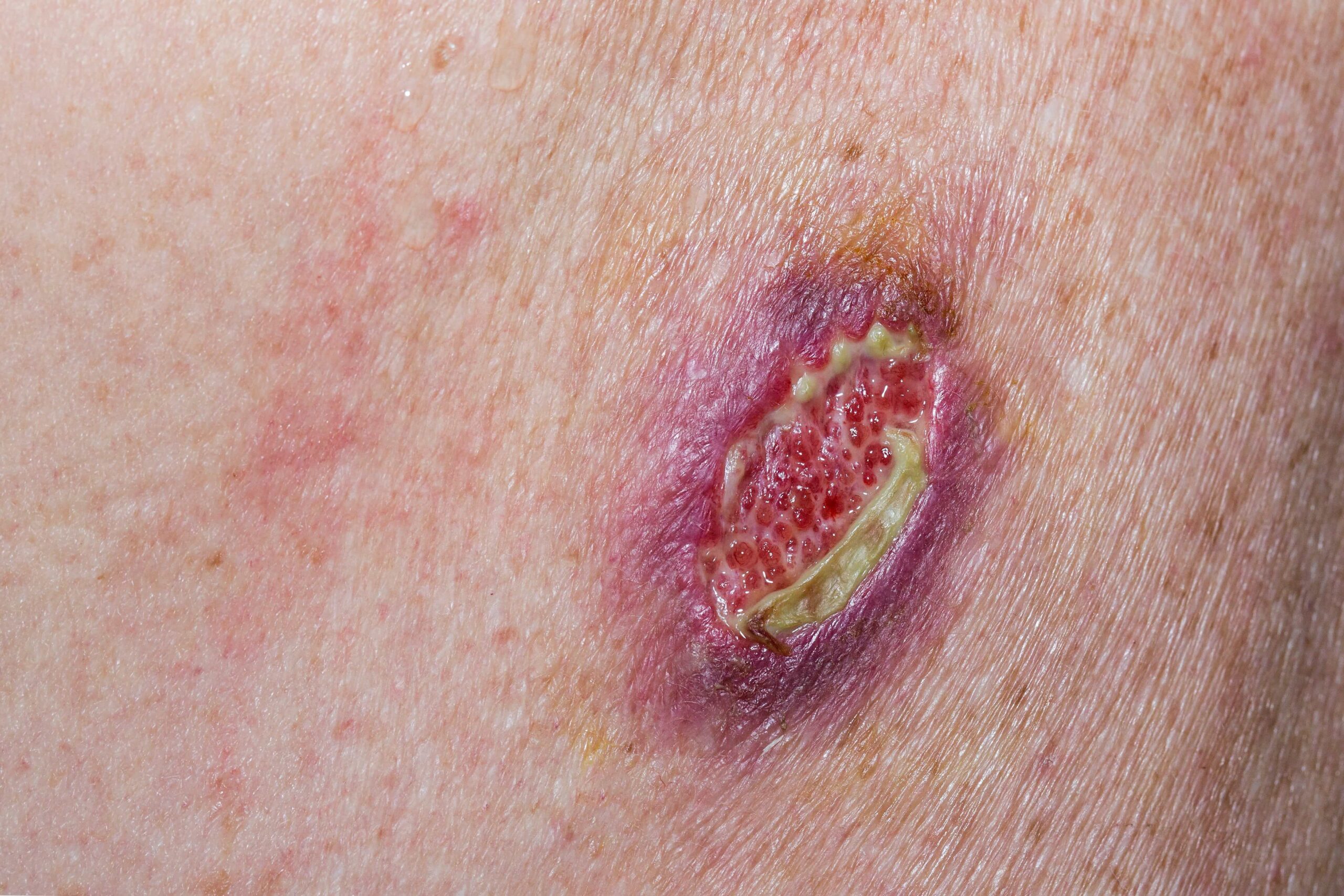
Signs and Symptoms
One of the most noticeable signs is the visible separation of the wound, which may range from a small opening to a complete reopening. Patients often experience increased pain or tenderness at the site, sometimes beyond what would be expected during normal recovery.
Swelling around the incision is also common, as the body reacts to the disruption. In some cases, fluid such as blood or pus may drain from the wound, which can indicate infection.
An unpleasant odor coming from the site is another warning sign that should not be ignored. Any combination of these symptoms should prompt immediate medical attention.
Causes and Risk Factors
Surgical technique plays a role, as inadequate closure or tension on the wound edges can make separation more likely.
Infection is one of the most common causes, weakening tissue and disrupting the healing process.
Patient-related factors also increase risk. Obesity can place additional pressure on the wound, while poor nutrition limits the body’s ability to repair tissue effectively.
Chronic conditions such as diabetes or cardiovascular disease may slow healing by reducing blood flow and impairing immune response.
Smoking further complicates recovery by restricting oxygen delivery to tissues. In addition, the use of certain medications, such as corticosteroids, can weaken the body’s natural healing mechanisms.
Wound Dehiscence Types
Wound dehiscence is generally classified based on the extent of the separation. Partial dehiscence involves only a portion of the wound reopening, while the rest remains intact.
Complete dehiscence is more severe, with full separation of the wound edges and exposure of underlying tissue layers. The severity of the condition often determines the level of treatment required.
Potential Complications
If left untreated, wound dehiscence can lead to several complications. Infection is one of the most immediate concerns, as open tissue is more susceptible to bacteria.
Healing may be significantly delayed, extending recovery time and increasing discomfort. In some cases, excessive or more noticeable scarring may develop.
For patients recovering from abdominal surgery, there is also a risk of hernia formation, where internal organs push through weakened tissue. This can create additional health issues that may require surgical correction.
Wound Dehiscence vs. Evisceration
Wound dehiscence is not synonymous with evisceration, a more severe and urgent condition. Evisceration occurs when internal organs protrude through the reopened wound. This is a medical emergency that requires immediate surgical treatment to prevent life-threatening complications.
While not all cases of dehiscence progress to evisceration, prompt care is essential to prevent escalation. Our centers as well as our mobile wound care can help.
Treatment Options
Treatment for wound dehiscence depends on how severe the separation is and whether infection is present. Mild cases may be managed with careful wound care, including cleaning, dressing changes, and close monitoring. Antibiotics may be prescribed if there are signs of infection or a high risk of developing one.
More severe cases often require surgical intervention. This may include debridement, a procedure in which damaged or infected tissue is removed to promote healthy healing.
After the area is properly cleaned, the wound may be re-closed using sutures or other techniques. A comprehensive evaluation of the patient’s overall health is often part of treatment to address underlying conditions that may have contributed to the issue.
Healing Timeline
The time it takes for a wound to heal after dehiscence varies widely. Minor cases may resolve within a few weeks with proper care, while more severe cases can take several months. Factors such as the patient’s overall health, the location of the wound, and adherence to treatment recommendations all influence recovery time.
Prevention Strategies
Reducing the risk of wound dehiscence begins with proper post-operative care. Following all medical instructions after surgery is essential, including keeping the wound clean and protected. Maintaining a balanced diet rich in protein, vitamins, and essential nutrients supports tissue repair and healing.
Avoiding smoking before and after surgery can significantly improve outcomes by enhancing blood flow and oxygen delivery. Managing chronic health conditions, such as diabetes, also plays a critical role in reducing risk.
Patients should avoid heavy lifting and strenuous activity during recovery, as excessive strain can place stress on the wound. Regular monitoring of the incision allows for early detection of any changes that may require medical attention.
If you notice any signs of wound separation or unusual symptoms during recovery, seeking professional wound care as soon as possible can make a meaningful difference in both short-term outcomes and long-term health.

What causes wound dehiscence?
Wound dehiscence can result from factors such as infection, poor surgical technique, or excessive tension on the wound. Certain patient-related conditions, including obesity, poor nutrition, diabetes, cardiovascular disease, and smoking, can increase the risk. Additionally, medications like corticosteroids may weaken the body’s ability to heal properly.
How is wound dehiscence treated?
Treatment depends on the severity of the wound separation and whether infection is present. Mild cases may be managed with proper wound care, including cleaning, dressing changes, and possibly antibiotics. More severe cases may require surgical procedures such as debridement and re-closure of the wound to promote healing.
How can wound dehiscence be prevented after surgery?
Prevention involves following post-operative care instructions carefully, including keeping the wound clean and avoiding unnecessary strain. A healthy diet, smoking cessation, and proper management of chronic conditions can support healing. Regular monitoring of the incision helps detect early warning signs so they can be addressed promptly.

