When blood sugar levels remain elevated, the body’s natural repair systems become less effective, increasing the risk of infections, chronic wounds, and serious complications. Wound healing with diabetes can present many challenges. However, with the right approaches, those challenges can be overcome.
Why is wound healing with diabetes slower?
Wound healing with diabetes is slower because high blood sugar levels reduce circulation, weaken the immune system, and prolong inflammation. These factors make it harder for the body to repair damaged tissue efficiently.
What are the most common types of diabetic wounds?
The most common diabetic wounds include foot ulcers, pressure sores, and minor cuts or blisters that fail to heal properly. Foot ulcers are especially common due to neuropathy and reduced sensation.
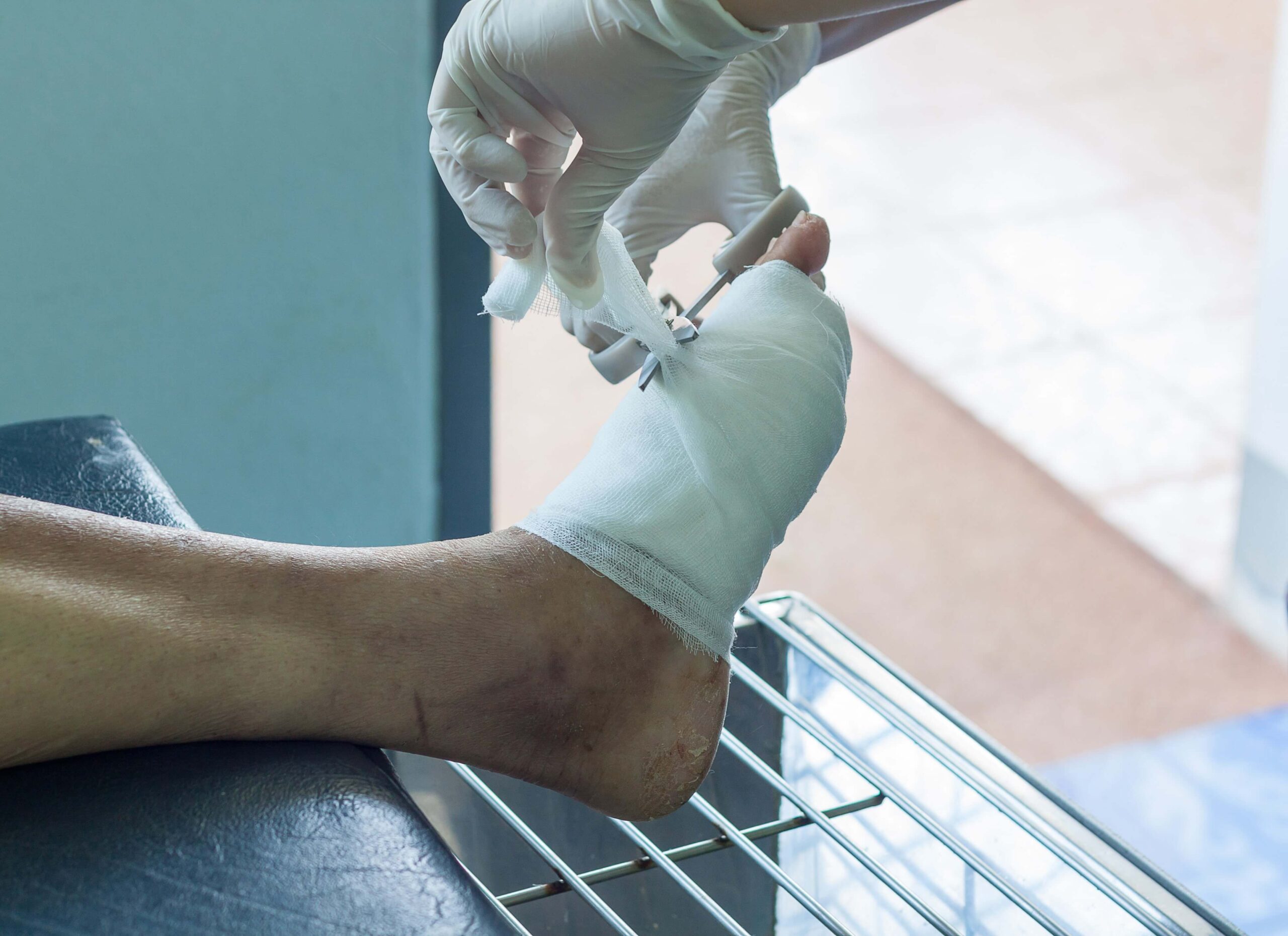
How Diabetes Interferes With Wound Healing
Diabetes affects several systems in the body at once, which is why healing becomes slower and less predictable. You can learn more about it from the NIH.
Chronic Inflammation
People with diabetes frequently experience prolonged inflammation. Instead of progressing to the next stage, wounds may remain stuck in the inflammatory phase for weeks or even months. This leads to chronic wounds that are harder to treat.
Elevated Blood Sugar Levels
High glucose levels create an environment that slows repair and encourages bacterial growth. This can:
- Reduce oxygen delivery to tissues
- Limit nutrient absorption
- Increase overall inflammation
- Delay the formation of new tissue
When blood sugar is not well managed, wound healing with diabetes becomes even more difficult.
Neuropathy (Nerve Damage)
Diabetic neuropathy can reduce sensation, especially in the feet. As a result:
- Minor cuts or blisters may go unnoticed
- Pressure injuries can worsen without detection
- Small wounds can develop into serious ulcers
Tip: Check your feet daily and wear properly fitted shoes to reduce risk.
Poor Circulation
Diabetes can cause blood vessels to narrow and harden, limiting circulation. Without proper blood flow:
- Oxygen delivery is reduced
- Nutrients cannot reach the wound effectively
- Tissue repair slows significantly
Poor circulation is one of the leading reasons wound healing with diabetes takes longer.
Weakened Immune Response
High blood sugar weakens white blood cells, making it harder for the body to fight infection. This increases the likelihood of complications and slows recovery.
Increased Risk of Infection
Because of slower healing and a compromised immune system, infections are more common and more severe. Without proper care, this can lead to:
- Skin infections
- Ulcers
- Gangrene
- In extreme cases, amputation
How the Body Heals Wounds
Wound healing is a structured biological process that occurs in four stages:
- Hemostasis
- Blood clotting begins immediately after injury to stop bleeding.
- Platelets form a protective barrier over the wound.
- Inflammation
- White blood cells move in to fight bacteria and remove debris.
- Mild swelling and redness are normal during this phase.
- Proliferation
- New tissue, blood vessels, and collagen develop.
- The wound starts to contract and fill in.
- Remodeling
- Skin strengthens and fully closes.
- Scar tissue forms as the wound matures.
For individuals without underlying health concerns, this process typically progresses smoothly. However, wound healing with diabetes often becomes delayed or disrupted at multiple stages.
In some cases, mobile wound care services allow patients to receive treatment at home, making it easier to stay consistent with care and avoid complications.
Preventing and Treating Diabetic Wounds
Daily Prevention Tips
- Inspect your skin every day, especially your feet
- Keep skin clean and moisturized
- Avoid walking barefoot
- Wear supportive, well-fitting footwear
- Manage blood sugar levels consistently
At-Home Wound Care Basics
- Clean wounds gently with appropriate solutions
- Keep wounds covered with sterile dressings
- Avoid putting pressure on affected areas
- Use prescribed topical treatments as directed
Lifestyle Factors That Support Healing
- Maintain a balanced, nutrient-rich diet
- Stay physically active to improve circulation
- Avoid smoking, which restricts blood flow
- Stay hydrated to support skin health
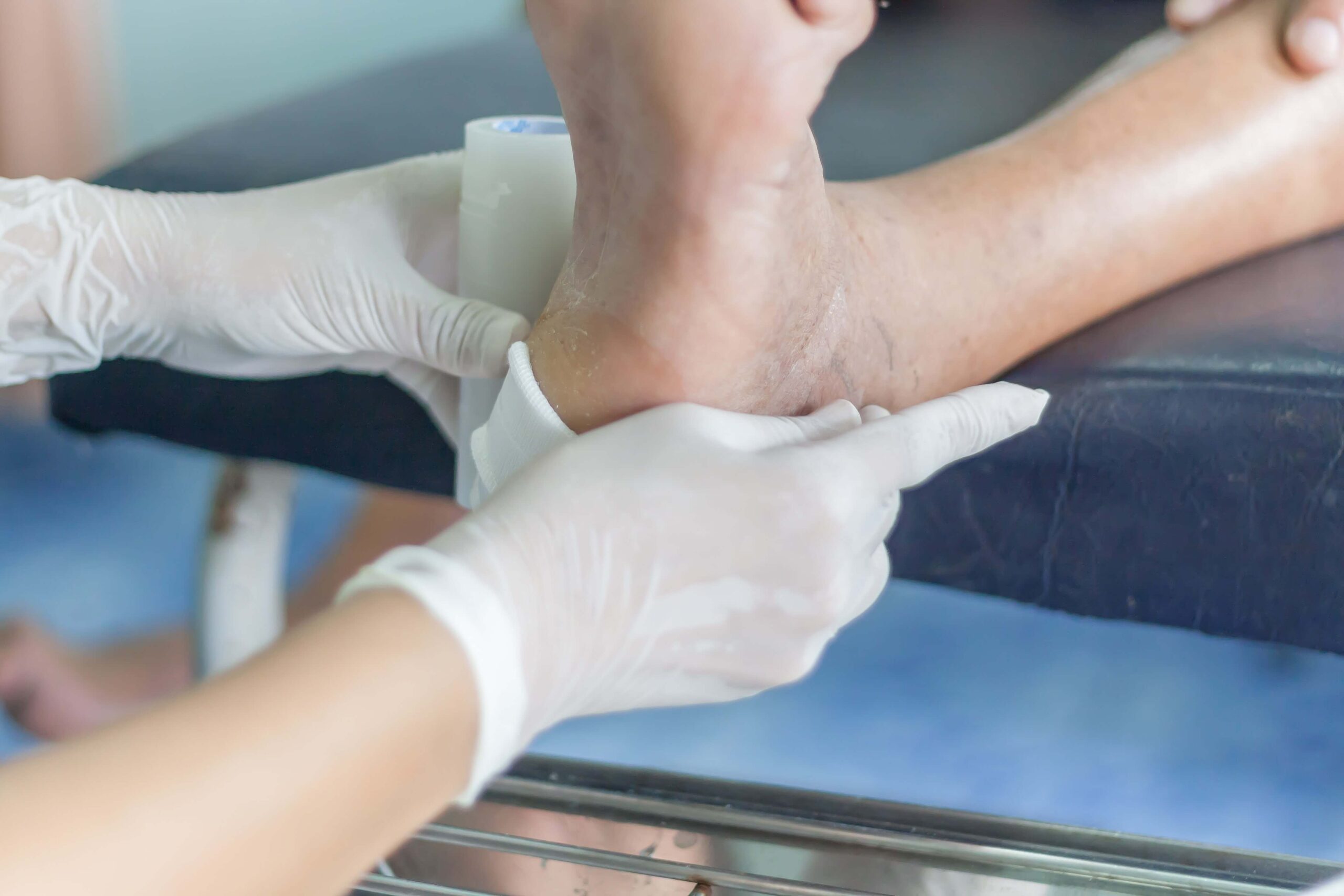
Advanced Care for Better Outcomes
For many patients, professional care is necessary to ensure proper healing. A wound care specialist team can provide targeted treatments that go beyond basic care.
These services may include:
- Debridement: Removal of dead or infected tissue
- Advanced dressings and skin substitutes
- Infection management
- Circulation therapies
- Personalized care plans
A Holistic Approach to Healing
Addressing wound healing with diabetes requires more than just treating the wound itself. A holistic wound care approach considers the full picture, including:
- Blood sugar control
- Nutrition and hydration
- Circulatory health
- Skin protection
- Infection prevention
When all of these factors are managed together, outcomes improve and healing times can be reduced.
Specialized Support for Wound Healing With Diabetes
Not all wounds can be treated at home. Seek medical attention for wound healing with diabetes if you notice:
- A wound that isn’t improving after a few days
- Increased redness, swelling, or warmth
- Drainage, odor, or discoloration
- Pain or numbness around the wound
Early intervention is crucial to preventing complications and supporting faster wound healing.
If you or a loved one is dealing with a slow-healing wound, seeking professional care can make a meaningful difference in recovery and long-term health.
Wound Healing With Diabetes FAQs
How can I prevent wounds if I have diabetes?
Daily skin checks, proper foot care, wearing well-fitting shoes, and maintaining stable blood sugar levels are important steps. Avoid walking barefoot and address even small injuries right away to prevent complications.
When should I see a specialist for a diabetic wound?
You should seek professional care if a wound shows no improvement within a few days, becomes painful, or shows signs of infection such as redness, swelling, or drainage. Early treatment can prevent serious complications.
What treatments help improve wound healing with diabetes?
Effective treatments include proper wound cleaning, dressings, debridement, infection control, and improved blood sugar management. Working with a wound care specialist team ensures a more comprehensive and targeted approach to healing.
