Osteomyelitis is a serious bone infection that can occur due to bacterial or fungal invasion. It can cause significant damage to the bone and surrounding tissue. Potentially, it can even lead to chronic bone infections, bone death, or amputation.
However, Osteomyelitis can be effectively treated. Full recovery is possible.
Osteomyelitis: In Greater Detail
As explained by the NIH, osteomyelitis is an infection of the bone. Usually, it is caused by bacteria, fungi, or other pathogens.
Infection may start in the bone itself after an injury. Additionally, infections could spread from surrounding tissue or through the bloodstream to the bone.
Osteomyelitis can occur in any bone in the body. It is most commonly found in the long bones of the arms and legs, in addition to the spine and pelvis.
Additionally, the most common bacteria that can result in osteomyelitis are Staphylococcus aureus, which is found on the skin and in the nose.
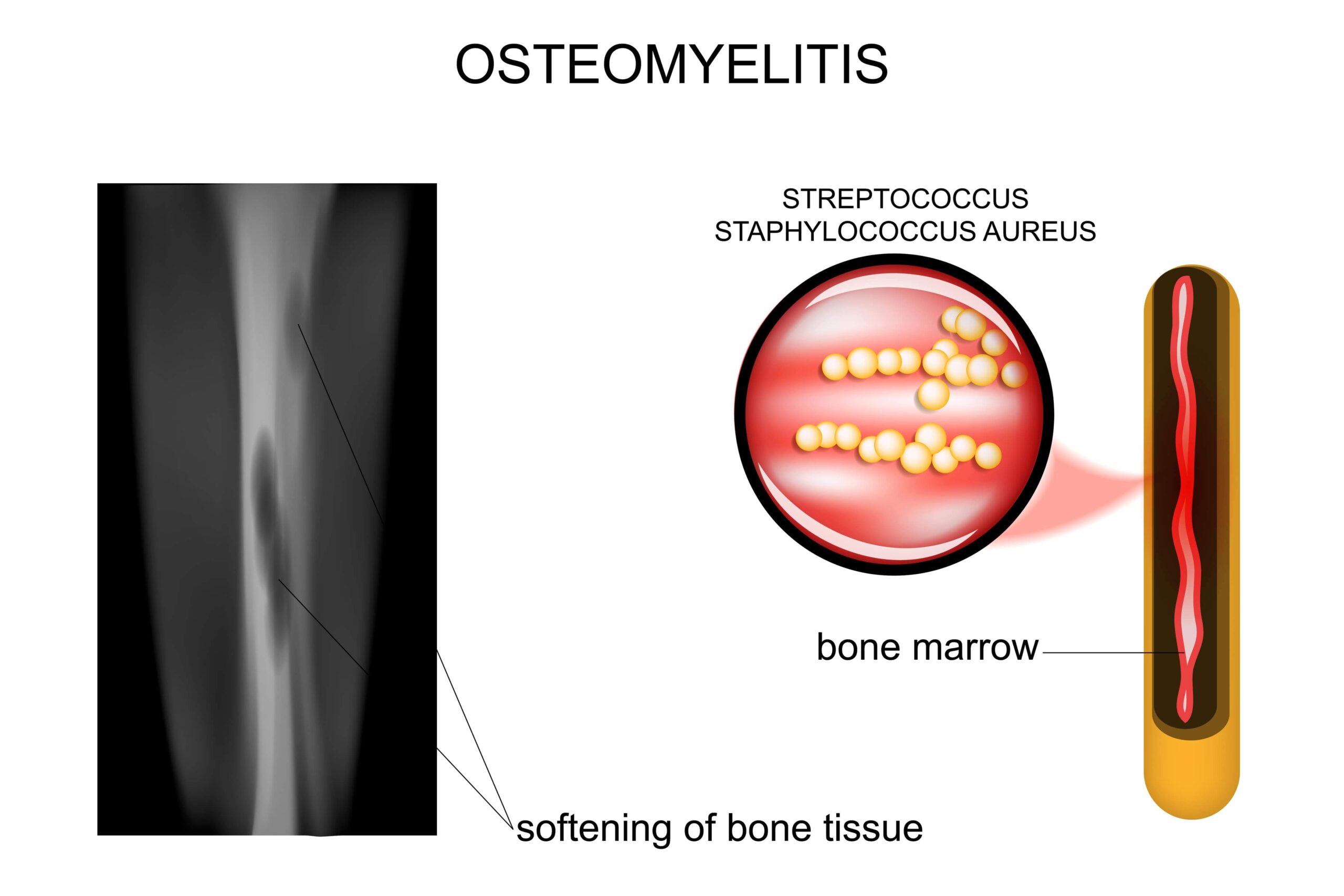
What is osteomyelitis?
It’s an infection of the bone caused by bacteria, fungi, or other pathogens. It can begin directly in the bone after an injury or spread from nearby tissue or through the bloodstream. The condition can affect any bone but is most commonly found in the arms, legs, spine, and pelvis.
What are the common symptoms of osteomyelitis?
Symptoms can vary depending on the severity of the infection and may include fever, nausea, swelling, redness, and pain in the affected area. Some people may also experience limited movement, drainage, or back pain if the spine is involved. In certain cases, osteomyelitis may present with no noticeable symptoms at all.
Treatment usually involves antibiotics to eliminate the infection and, in some cases, surgery to remove damaged bone tissue. Additional care, such as proper wound management and addressing underlying conditions, plays an important role in healing. With timely and appropriate treatment, be it in a center or our mobile wound care, full recovery is possible.
Osteomyelitis Symptoms
Symptoms vary depending on the type and severity of the infection. Symptoms can include:
- Fever
- Nausea and vomiting
- Swelling and redness around the affected area
- Pain and tenderness in the affected bone
- Limited movement or stiffness in the affected joint
- Drainage from the affected area
- Stiff back or lower back pain (if vertebrae are affected)
If you are experiencing any of these symptoms, it is essential to visit a wound care center as soon as possible.
Osteomyelitis Diagnosis
Following a physical examination, wound specialists may conduct blood tests, imaging tests, and in some cases, bone biopsies.
Blood tests can help detect inflammation and signs of infection. In isolation, a blood test might not be able to determine definitively if you have Osteomyelitis. However, a blood test can help your specialist determine what follow up tests might be needed.
Imaging tests help identify the infection’s location and severity.
A bone biopsy can determine what type of infection you have. This can help in identifying the correct course of treatment.

Osteomyelitis Risk Factors
Young children, the elderly, and people with certain circulatory conditions are at a higher risk of developing osteomyelitis.
Conditions that can increase the risk of osteomyelitis:
- Compromised Immune System
- Diabetes
- Intravenous Drug Use
- Recent Surgery
- Deep puncture wounds or bone fractures
Osteomyelitis Types
There are two main types of osteomyelitis: acute and chronic.
Acute osteomyelitis is a sudden and severe infection.
Chronic osteomyelitis can last for months or even years.
Osteomyelitis Treatments
Treatment typically involves a combination of antibiotics and surgery. Antibiotics are used to eliminate the infection, while surgery may be necessary to remove any dead or infected bone tissue.
The type of antibiotics used will depend on the severity of the infection and the bacteria or fungus causing it.
In some cases, bone grafts may also be necessary to help the bone heal.
In addition to antibiotics and surgery, it is important to practice proper wound care and management to prevent the infection from spreading. This can include keeping the affected area clean and dry, changing dressings regularly, and avoiding any activities that could cause further injury. Your wound care specialist can outline a plan and recommendations for you to follow as you heal.
Additionally, it can be important to follow your specialist’s recommendations for treating any underlying conditions that could impair healing.
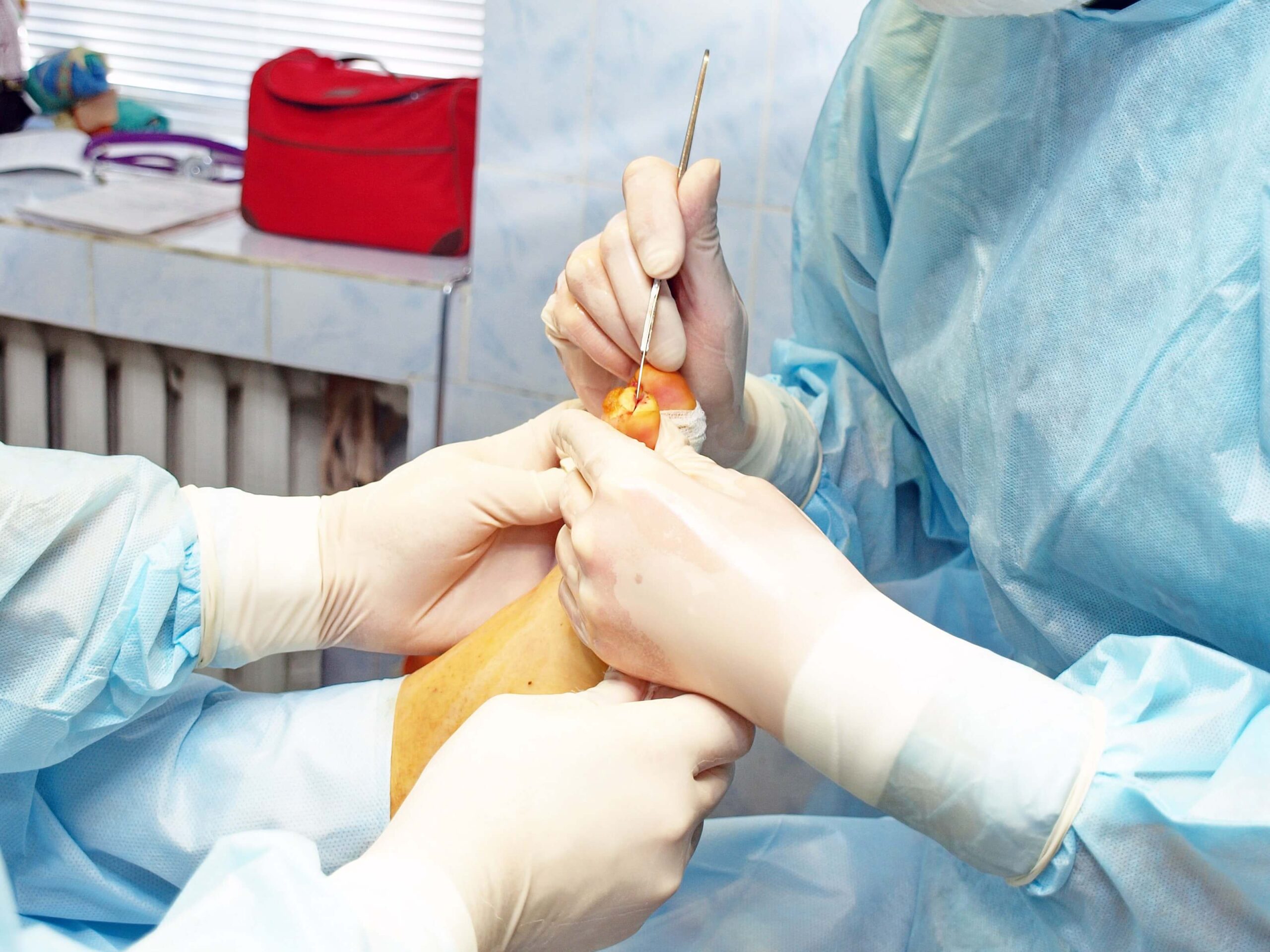
Recovery for Osteomyelitis is Possible
If you suspect you may have osteomyelitis or are experiencing symptoms, it’s imperative to seek professional help. The sooner the condition is diagnosed and treated, the better the outcome and the faster you can get back to normal activity.
How is osteomyelitis diagnosed?
Diagnosis typically begins with a physical exam followed by blood tests to identify signs of infection or inflammation. Imaging tests are often used to locate the infection and determine its severity. In some cases, a bone biopsy is performed to identify the exact cause and guide treatment.
Who is at high risk for developing osteomyelitis?
Young children, older adults, and individuals with compromised immune systems or circulatory conditions face a higher risk. Diabetes, recent surgery, deep wounds, and intravenous drug use can also increase susceptibility. These factors can make it easier for infections to enter the body and spread to the bone.

