[fusion_builder_container hundred_percent=”no” equal_height_columns=”no” menu_anchor=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” background_color=”” background_image=”” background_position=”center center” background_repeat=”no-repeat” fade=”no” background_parallax=”none” parallax_speed=”0.3″ video_mp4=”” video_webm=”” video_ogv=”” video_url=”” video_aspect_ratio=”16:9″ video_loop=”yes” video_mute=”yes” overlay_color=”” video_preview_image=”” border_color=”” border_style=”solid” padding_top=”” padding_bottom=”” padding_left=”” padding_right=”” type=”legacy” admin_toggled=”no”][fusion_builder_row][fusion_builder_column type=”2_3″ layout=”1_1″ background_position=”left top” background_color=”” border_color=”” border_style=”solid” border_position=”all” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” center_content=”no” last=”false” min_height=”” hover_type=”none” link=”” border_sizes_top=”” border_sizes_bottom=”” border_sizes_left=”” border_sizes_right=”” first=”true” spacing_right=”2.6666666666666665%”][fusion_text columns=”” column_min_width=”” column_spacing=”” rule_style=”default” rule_size=”” rule_color=”” content_alignment_medium=”” content_alignment_small=”” content_alignment=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” sticky_display=”normal,sticky” class=”” id=”” margin_top=”” margin_right=”” margin_bottom=”” margin_left=”” font_size=”” fusion_font_family_text_font=”” fusion_font_variant_text_font=”” line_height=”” letter_spacing=”” text_color=”” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=””]
If you have diabetes, your body functions a bit differently than people who don’t have diabetes. As a diabetic, your body either does not produce insulin naturally, or is unable to use it properly. This may lead to the need to test your blood sugar often and use artificial insulin. However, it also means that wounds might not heal as quickly or effectively as they would in a body without diabetes.
If you or someone you know is suffering from diabetes, it’s crucial to understand how it can affect wound healing and be aware of the importance of proper wound care and management. Diabetic wounds that are not taken care of can quickly progress into an infection which can result in serious complications such as required surgery, foot ulcers, or even amputation.
Generally, there are four stages of wound healing:
The foundation for new tissue is red blood cells. These blood cells then create collagen, which in turn becomes new tissue. Once this new tissue is formed it leads to new skin growing over the tissue. At the point that the wound finally heals, the edges then pull inward and the wound will begin to get smaller.
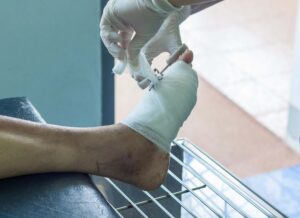 Unfortunately, Diabetes is a common problem in this country. In fact, according to recent data from the Centers for Disease Control and Prevention (CDC) 28.7 million people in the United States have been diagnosed with diabetes. Due to the nature of the disease, many of these individuals will develop wounds that heal slowly, improperly, or won’t heal at all. Without proper medical attention, this can result in wound infection among other serious health issues.
Unfortunately, Diabetes is a common problem in this country. In fact, according to recent data from the Centers for Disease Control and Prevention (CDC) 28.7 million people in the United States have been diagnosed with diabetes. Due to the nature of the disease, many of these individuals will develop wounds that heal slowly, improperly, or won’t heal at all. Without proper medical attention, this can result in wound infection among other serious health issues.
Let’s take a look at how diabetes impacts wound healing, how the disease makes the recovery process more difficult, and what you can do to help if you or a loved one is diabetic and has suffered a serious wound.
During the second stage of healing, wounds are inflamed. However, when diabetic wounds heal, sometimes this stage can take too long; resulting in the wound becoming “chronic”. A wound is considered chronic when it lasts for six months or longer.
Because diabetes limits the body from handling glucose, one of the most important things that diabetics need to worry about is maintaining a healthy blood sugar level. Blood sugar levels are a major determining factor in how efficiently your wounds heal. When these levels are too high, in people with diabetes, for example, it can interfere with how the immune system functions, prevent nutrients and oxygen from energizing cells, and increase inflammation. All of which, can interfere with efficient wound healing.
High blood glucose can also cause the arteries to become stiff, which can lead to narrow blood vessels and diabetic neuropathy. Diabetic neuropathy occurs when nerves become damaged all over the body. It causes tingling and numbness in the limbs, which makes it difficult to be aware of whether or not you are injured. This can lead to new wounds and complications in overall healing.
In light of that, it’s important for diabetics to check their skin often, especially the bottom of the feet. The legs and feet are most commonly affected by diabetic neuropathy.
Additional Tip: People who suffer from diabetic neuropathy should ensure they wear shoes that fit properly and avoid cuts, blisters, and any type of activity that may cause ulcers.
Wounds heal much quicker when there is a good circulation of blood throughout the body. Diabetics typically have poor circulation due to narrowed blood vessels and are more likely to develop poor circulation conditions like peripheral vascular disease. The reduced oxygen in those suffering from diabetes can result in slower tissue development and in turn, wound healing.
High blood sugar levels decrease red and white blood cell function, which reduces nutrients being sent to the wound site to fight infections. This is also due to a diabetic body producing certain hormones that make the immune system less effective. If your immune system isn’t functioning correctly, it can slow wound healing and because the body can have a difficult time fighting off bacteria it can put you at greater risk of infection.
Additional Tip: Some doctors recommend wearing white socks at all times in order to be able to see any blood or pus if an injury occurs. This can help alert you if there are cuts, blisters, or another type of wound.
Diabetic patients have a slower movement of white blood cells than the average person. This means that there is less of an immune response, which leaves wounds to be more inflamed. This combined with numbness from neuropathy can lead to the wound getting worse.
As referenced above, with an open wound that heals slower than it normally would, there is an increased chance of infection. This often leads to higher rates of gangrene, sepsis, and infections like osteomyelitis. Out of all of the limbs amputated each year, diabetic ulcers are the number one cause.
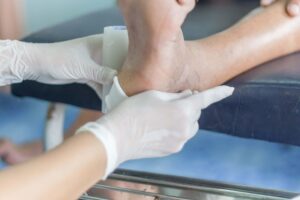 If not carefully monitored and treated, wounds can be very serious and quickly lead to infection. Fortunately, wound care specialists are trained and equipped with the expertise to help ensure wounds are cared for properly and healed efficiently. If you get a diabetic ulcer or are unsure of a wound it’s important to see a medical professional as soon as possible. Especially if the wound isn’t healing or infection has started to spread.
If not carefully monitored and treated, wounds can be very serious and quickly lead to infection. Fortunately, wound care specialists are trained and equipped with the expertise to help ensure wounds are cared for properly and healed efficiently. If you get a diabetic ulcer or are unsure of a wound it’s important to see a medical professional as soon as possible. Especially if the wound isn’t healing or infection has started to spread.
Your wound care specialist will work with you to help prevent the wound from getting bigger and avoid potential infection. They may also conduct debridement which helps remove unhealthy tissue from the wound and facilitate healing.
While most diabetic wounds are better addressed through a specialist, there are a few steps you can take to help the recovery process and even prevent wounds from surfacing:
Wounds can become serious for anyone but it’s even more important for those with diabetes to stay vigilant and ensure you are caring for them properly. If you or a loved one believes they might have a diabetic wound, the wound care specialists at West Coast Wound & Skin Care are here to help. We provide high quality, full spectrum wound care services to patients wherever they reside.
We Heal Diabetic Ulcers 25% Quicker Than Other Practices!
We also welcome you to come visit our new Wound Center in Fresno where our wound care physicians help treat the complete range of wound types and skin concerns including diabetic wounds and ulcers. Contact us today to book an appointment and let us help you get on the path to recovery.
[/fusion_text][/fusion_builder_column][fusion_builder_column type=”1_3″ layout=”1_3″ spacing=”” center_content=”no” link=”” target=”_self” min_height=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” hover_type=”none” border_color=”” border_style=”solid” border_position=”all” border_radius=”” box_shadow=”no” dimension_box_shadow=”” box_shadow_blur=”0″ box_shadow_spread=”0″ box_shadow_color=”” box_shadow_style=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” margin_top=”” margin_bottom=”” background_type=”single” gradient_start_color=”” gradient_end_color=”” gradient_start_position=”0″ gradient_end_position=”100″ gradient_type=”linear” radial_direction=”center center” linear_angle=”180″ background_color=”” background_image=”” background_image_id=”” background_position=”left top” background_repeat=”no-repeat” background_blend_mode=”none” animation_type=”” animation_direction=”left” animation_speed=”0.3″ animation_offset=”” filter_type=”regular” filter_hue=”0″ filter_saturation=”100″ filter_brightness=”100″ filter_contrast=”100″ filter_invert=”0″ filter_sepia=”0″ filter_opacity=”100″ filter_blur=”0″ filter_hue_hover=”0″ filter_saturation_hover=”100″ filter_brightness_hover=”100″ filter_contrast_hover=”100″ filter_invert_hover=”0″ filter_sepia_hover=”0″ filter_opacity_hover=”100″ filter_blur_hover=”0″ last=”true” border_sizes_top=”0″ border_sizes_bottom=”0″ border_sizes_left=”0″ border_sizes_right=”0″ first=”false” spacing_left=”1.3333333333333333%”][fusion_widget_area name=”avada-blog-sidebar” title_size=”” title_color=”” background_color=”” padding_top=”” padding_right=”” padding_bottom=”” padding_left=”” hide_on_mobile=”small-visibility,medium-visibility,large-visibility” class=”” id=”” /][/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]
The current 2025 government shutdown has introduced significant challenges across many sectors, with the healthcare industry feeling a considerable impact. For millions of Americans who rely on federal programs for their health needs, the shutdown caused instant concerns. At West Coast Wound Care, we will always provide high-quality advanced wound care to our patients.
We continue to accept Medicare and ensure patients receive needed treatment, regardless of disruptions in Washington. During times of uncertainty, consistency in healthcare is more important than ever.
A government shutdown occurs when funding for federal agencies expires, halting non-essential government operations. This has wide-ranging consequences for the healthcare system. Federal agencies like the Centers for Medicare & Medicaid Services (CMS) face hurdles, causing delays and confusion for providers and patients.
While mandatory programs like Medicare and Medicaid continue to operate, the strain causes delays and postponed billing updates. It can also create a general sense of instability.
It’s understandable that patients may worry if providers will still accept insurance or if care access will be compromised.
Medicare patients are particularly vulnerable during these periods. Many rely on Medicare for their healthcare coverage, and shutdown anxiety can be immense. Chronic wounds, which require consistent and specialized attention, cannot be put on hold. A delay in treatment can lead to severe complications, including infection, hospitalization, and a decreased quality of life.
For these individuals, reliable access to care is a critical health requirement. We understand. As such, our services are structured in such a way that we remain stable and dependable for those in need.
We want to assure our community that our commitment to patient care remains unchanged. A majority of the patients we serve are covered by Medicare, and our operations are designed to navigate the complexities of the system, even during a shutdown.
We continue to welcome new and existing Medicare patients at our clinics and through our mobile services.
Our billing and administrative teams manage Medicare claims and work diligently to prevent any potential disruptions. Your health is our top priority. We provide the same high standard of care you expect, without interruption.
We believe political struggles should not impede access to expert wound management. Our state-of-the-art wound care clinics are equipped with the latest technology and staffed by dedicated professionals. For patients in particular locations, our unique mobile wound care service brings our expertise directly to their homes or residential facilities.
This service is especially valuable for individuals with mobility issues or those who live in areas with limited access to specialized medical facilities. By offering both in-clinic and mobile options, we remove barriers to receiving timely and effective treatment, ensuring that all our patients can get the care they need, when and where they need it.
The healthcare landscape is constantly evolving, with a growing emphasis on value and quality over volume. A recent proposal from CMS, outlined in the Physician Payment Rule, aims to reduce wasteful spending and enhance quality measures. This proposal focuses on paying physicians for providing high-quality care that improves patient outcomes, rather than just for the number of services performed.
It signifies a shift toward a more patient-centered and efficient healthcare system, rewarding providers who prioritize effective treatments and positive results. This forward-thinking approach is designed to ensure that taxpayer dollars are used to support care that genuinely helps patients heal and stay healthy.
We responded to that particular article because, frankly, our entire model is built around delivering superior outcomes. Every patient receives a personalized treatment plan developed by a wound care specialist, designed to promote faster healing and prevent complications. We utilize the most effective and evidence-based methods in advanced wound care to ensure our patients achieve the best possible results.
Our focus has always been on the quality and efficacy of our treatments, not the quantity. We track patient progress closely, adjust plans as needed, and are committed to a standard of excellence that puts patient well-being first. This commitment to quality care ensures that we are not only meeting current standards but are also well-prepared for the future of healthcare.
Navigating the healthcare system can be challenging, and the uncertainty of a government shutdown only adds to the stress. If you or a loved one is dealing with a chronic or non-healing wound, delaying treatment is not an option.
Your health and healing are too important to be put on hold. We are here to provide the support and expert medical attention you need, and we continue to proudly accept Medicare patients.
Let us help you get on the path to recovery. Reach out to our team today to schedule a free appointment.
Peripheral Arterial Disease (PAD) affects millions of people and can severely impact wound healing, especially when blood flow to the limbs is compromised. Every year, more awareness is needed so that individuals recognize early signs and get care that prevents complications. We believe in empowering patients during PAD Awareness Month—and beyond—by providing comprehensive wound care services that address not just symptoms, but root causes that interfere with healing.
PAD reduces blood flow through arteries, especially to the feet and legs. When circulation is impaired, tissues receive less oxygen and fewer nutrients, which slows healing. Arterial ulcers are one of the most serious wound types associated with PAD. These are often deep, painful, and slow to respond to treatment. Infections can set in, risking more severe outcomes.
People with PAD may also have coexisting conditions—like diabetes, kidney disease, or hypertension—that further complicate recovery. Recognizing PAD early means we can intervene with treatments that restore or improve circulation, manage risk factors, and prevent ulcers from worsening.
As a patient‐facing wound care provider, we focus on therapies supported by clinical evidence and tailored to the needs of those living with PAD. Here are the main treatments we deliver:
These treatments are available both at our wound care clinics and through our mobile services. When surgical or specialty procedures are needed, we help patients coordinate referrals and follow up to ensure healing proceeds well through our comprehensive wound care services.
We provide care through multiple settings so that individuals with PAD get help in the way that works best for them.
At these clinics we offer advanced treatments such as negative‐pressure wound therapy (NPWT), hyperbaric oxygen therapy (HBOT), and debridement procedures. These help wounds heal more quickly and reduce complications.
For patients with mobility or distance challenges, we provide mobile wound care through our comprehensive wound care services.
We bring our expert team of physicians, nurse practitioners, and wound care specialists to private homes, assisted living facilities, board and care homes, and skilled nursing facilities. This allows us to deliver treatments like dressing changes, infection control, and monitoring without requiring the patient to travel.
An early diagnosis of PAD can make a major difference. When wounds are detected early, before infection or tissue death sets in, our outcomes are much better. During PAD Awareness Month, we encourage:
In our care model, once a PAD‐related wound is identified, we schedule frequent follow‐ups either through mobile or clinic‐based visits, monitor for signs of breakdown, manage infections, and adjust treatment based on healing progress. These follow-ups are key components of our comprehensive wound care services.
PAD Awareness Month is a reminder—but we offer support beyond that. Our services are structured so that patients with PAD can count on:
We accept Medicare and many insurance plans so that financial barriers are minimized.
PAD need not lead to permanent wounds or loss of mobility. With early recognition, strong clinical intervention, and the right healing environment, it is possible to avoid many of the worst outcomes. We are here for you: through our wound care clinics, through mobile wound care, and through committed, evidence‐based wound care services, we strive to heal wounds faster, reduce suffering, and restore quality of life.
If you or someone you love is living with PAD and noticing wounds that aren’t healing, reach out to us. Our team of dedicated professionals is ready to provide care that makes a meaningful difference.
When wounds resist healing because of infection, poor circulation, or chronic disease, the right medical approach can make the difference between slow recovery and meaningful healing. At West Coast Wound & Skin Care, our advanced wound care centers offer advanced infusion and IV therapy as integral parts of our comprehensive treatment offerings. We bring together highly trained providers, modern medical technology, and compassionate care so that you get the best support tailored to your wound’s unique needs.

Infusion therapy means delivering medications, antibiotics, or other healing agents directly into the bloodstream over time, while IV therapy refers more broadly to intravenous delivery of fluids, electrolytes, and medications.
These methods are especially helpful in situations where oral medication might be insufficient—such as when a wound is deeply infected, the patient’s digestive absorption is impaired, or systemic support (hydration, nutrition) is required to promote healing.
We rely on wound care specialists who assess multiple factors: wound depth and type, presence of infection, blood flow, patient overall health (e.g., kidney function, heart health), allergies, and potential interactions with other treatments. When an IV antibiotic or another infused agent is needed, we administer it under sterile conditions, monitor for side effects, adjust dosing as needed, and coordinate with other therapies like debridement, dressings, or hyperbaric oxygen (if available at your advanced wound care centers).
One of the greatest benefits when treating infected wounds is that infusion and IV therapy allow medications to reach high tissue levels quickly. This means:
This is especially valuable for patients with vascular compromise, diabetes, or weakened immune systems, since they often face tougher challenges overcoming infection.
Wounds heal best when the body has adequate hydration, proper electrolyte balance, and sufficient nutrition. IV fluids can correct dehydration or electrolyte imbalances. In certain cases, infusions can include components—such as minerals, vitamins, or growth-factors—when indicated by bloodwork and medical need. This systemic support helps the body mount the correct response: generating new tissue, fighting microbes, and closing wounds more efficiently, especially when provided through advanced wound care centers.
Infusion and IV therapies work best in combination with our other services. While the IV approach works on internal systemic issues, our clinic-based services handle local problem areas: cleaning, dressing selection, debridement, pressure relief, and advanced local therapies. By coordinating the systemic with the local, healing proceeds more smoothly, with fewer setbacks.
Our wound care clinics offer:
These clinic-based services ensure that patients who can travel have access to full medical support in a controlled, well-equipped environment.
Not everyone is able to come into one of our clinics. For those individuals, our mobile wound care service comes to your home, or to your facility. While mobile settings may limit what we can infuse compared to the clinic, we provide:
This blended approach means you don’t lose access to high level infusions just because you can’t leave home.
We consider infusion or IV therapy when:
In these cases, access to advanced wound care centers ensures that the therapy is properly administered and monitored for effectiveness.
Administering IV therapy demands strict protocols. When you receive this therapy, we ensure:
Infusion and IV therapy in isolation are rarely sufficient. We pair them with:
This holistic care ensures the infused or IV agents are effective, not wasted by unresolved local issues.
If you believe you need infusion or IV therapy, or have a wound that isn’t healing, here’s how we help you begin:
Our wound care centers are places where advanced therapeutic modalities meet compassionate, individualized care. Infusion and IV therapy is not just giving a drug—it is delivering healing potential, accelerating recovery, reducing complications, and restoring your quality of life.
Whether you’re seen at a clinic or through mobile wound care, we ensure that our wound care specialist-led teams bring you the maximum benefit possible. If your wound has been stubborn, infected, or slow to heal, reach out to us for a free appointment.
Artificial intelligence (AI) is transforming healthcare (as well as so much else in life), and innovative wound care is no exception. As mobile and clinic-based care providers, we’ve seen firsthand how digital tools and data-driven innovations can improve accuracy, speed, and outcomes. AI, when used correctly, enhances every stage of wound treatment—from the moment of diagnosis to the final stages of healing. But no algorithm replaces a trained eye.
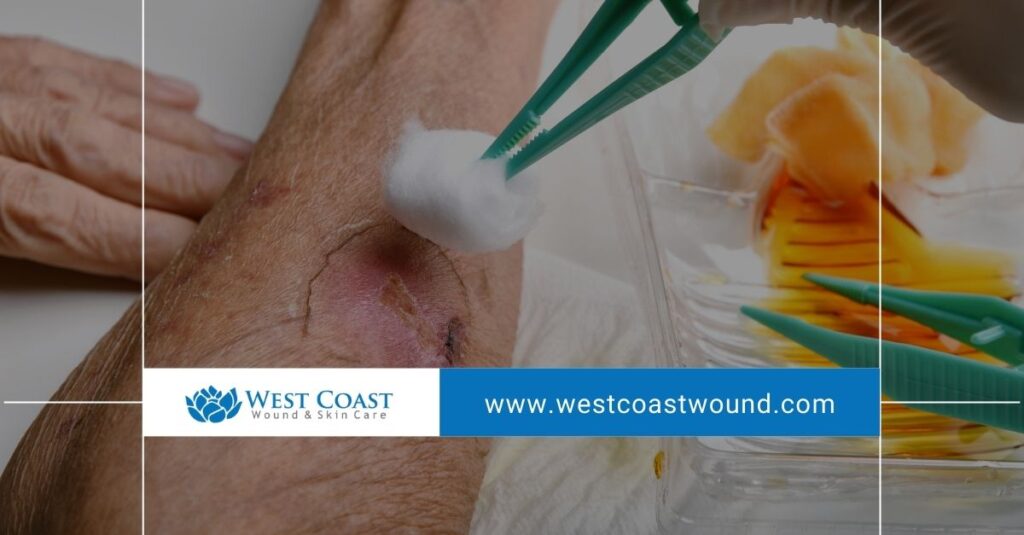
We would only ever potentially integrate artificial intelligence into our services with a clear priority: to better serve patients through greater precision, faster interventions, and a more personalized level of care. That said, we have noticed ways in which that AI is transforming healthcare.
Diagnosing a wound correctly is crucial to healing it effectively. AI-powered imaging platforms can analyze digital photographs or scans of wounds, measuring parameters like size, depth, and color. This shift is a cornerstone of innovative wound care, allowing clinicians to act with more precision and speed.
These platforms are trained on vast databases of wound images, allowing them to identify wound types—such as pressure injuries, venous ulcers, diabetic foot ulcers, and arterial wounds—with a surprising degree of accuracy.
In practice, AI helps us flag wounds that need immediate intervention. For example, AI tools can quickly detect early-stage tissue necrosis or signs of infection, which might otherwise be missed by an untrained eye. Some tools even assess wound margins, moisture levels, and granulation tissue quality—all of which provide insight into whether a wound is healing or deteriorating.
For mobile wound care services in particular, the speed of AI-aided diagnostics, if properly overseen by trained professionals, could be a great boon. That day isn’t here yet, but, we will continue to monitor the tech until it can.
AI doesn’t make decisions; it presents options and then, it can provide support for your eventual decisions. Machine learning models can compare a current wound against thousands of documented cases, offering likely outcomes based on past patient histories, treatments, and responses. These insights make innovative wound care not only more accurate but also more personalized for each patient.
This helps our providers make more informed recommendations about dressings, debridement schedules, or whether a referral to a specialist may be warranted.
When we combine AI analysis with patient-specific data—such as comorbidities, lifestyle, or previous wound history—we get a more nuanced understanding of each case. This means our team can avoid unnecessary interventions and focus on therapies most likely to succeed.
Healing a wound is a process. That process can stall for many reasons, from infection to poor circulation. AI helps us track that progress with greater precision. Instead of relying solely on manual measurements, we can use AI-driven wound imaging platforms that automatically measure changes in size, depth, and tissue appearance over time. This level of monitoring reflects the true value of innovative wound care in modern healthcare.
These automated tracking systems reduce human error and help us identify non-healing wounds earlier than we might otherwise. If a wound shows signs of stagnation, we can intervene with advanced therapies—like compression, negative pressure wound therapy, or enzymatic debridement—before complications develop.
This kind of progress monitoring makes follow-up visits more efficient and meaningful. It also keeps patients engaged, as we can show them visual, data-based proof of improvement.
AI adds another layer of precision, helping us craft care plans that respond to the unique challenges and goals of each patient. Based on this analysis, we may adjust a patient’s treatment plan to incorporate offloading strategies, nutritional counseling, or adjunctive therapies earlier in the process.
Some AI platforms even suggest wound dressing types based on wound stage, bacterial burden, and drainage levels. While our providers always make the final call, these suggestions can expedite decision-making and open up options we may not have considered otherwise.
AI offers powerful tools, but those tools require experienced clinicians to interpret, supervise, and apply the data effectively. A machine can detect signs of deterioration, but it can’t assess pain, hear patient concerns, or understand a patient’s personal goals. That’s the job of our trained wound care providers.
We don’t see AI as a substitute for human judgment. Instead, we see it as an enhancement—a digital second opinion that supports our team’s clinical intuition and medical training. Our providers may use AI as part of a broader ecosystem of care that includes bedside assessments, lab tests, and patient conversations.
With any digital tool, especially one involving sensitive health data, safety and ethics matter. We use HIPAA-compliant platforms and ensure that all AI-integrated technologies meet regulatory standards. Our providers are trained in how to interpret AI data properly and communicate those findings to patients in a clear, compassionate manner.
We also recognize the limitations of AI. No system is perfect, and even the most advanced algorithms can misinterpret a wound due to lighting, skin tone variations, or other visual distortions. That’s why all AI-derived data is reviewed by a qualified clinician before any clinical decisions are made.
At West Coast Wound and Skin Care, we’re committed to offering our patients the best possible outcomes—and that means using every effective tool at our disposal. AI has proven to be a powerful ally in both wound diagnosis and wound healing. Whether through our mobile services or at our clinics, West Coast Wound and Skin Care integrates AI into our workflow not to replace what we do, but to enhance it.
Our patients benefit from faster diagnoses, more accurate tracking, and treatment plans shaped by both data and clinical insight. And because West Coast Wound and Skin Care treats every patient as an individual, our use of AI is always adapted to fit the person, not the other way around.
From detecting complications early to adjusting care based on healing trends, artificial intelligence allows us to stay one step ahead. But no matter how advanced the software becomes, the providers at West Coast Wound and Skin Care remain at the heart of every decision, every visit, and every healing process. If you or someone you care for needs personalized, professional wound care backed by the latest technology, we’re here to help. You can schedule an appointment through our site.
Whether in a hospital setting, outpatient clinic, or mobile wound care environment, clinicians are expected to adhere to established standards that safeguard patient outcomes and legal accountability. Clear, timely, and accurate wound documentation is often the difference between resolving a dispute quickly or being drawn into a prolonged legal or regulatory process.
Below, we’ll explore how wound assessment documentation relates to professional liability, what providers need to consider in their daily practice, and how institutional policies can serve as protective mechanisms. Through vigilance and meticulous work, it’s possible to strengthen and maintain patient trust all while minimizing exposure to risk.
Wound care involves working with patients who often have compromised immune systems, chronic illnesses, or complex post-surgical conditions. These factors make wound healing more unpredictable and the margin for error much narrower. Any lapse in communication, delayed documentation, or failure to track progression accurately may lead to preventable complications.
In litigious or regulatory reviews, this (rightfully) puts the spotlight on how thoroughly care was documented.
Professional liability claims are commonly tied to:
When documentation falls short, even appropriate clinical decisions can be difficult to defend after the fact.
This is particularly true in a wound care environment where the margin for error is narrower.
Liability insurance for wound care providers typically protects against claims of negligence, omissions, or errors in care. These policies may cover legal defense fees, settlement costs, and damages awarded if a provider is found legally responsible. However, many policies have specific requirements related to clinical documentation. If those expectations are not met, insurers may reduce or deny coverage.
Some policies stipulate that care must be documented according to recognized clinical guidelines or facility protocols. Others may require that documentation be completed within a certain time frame after services are rendered. Providers unaware of these terms could unintentionally jeopardize their protection.
High-quality wound documentation helps show that the provider followed accepted standards of care, responded appropriately to changes in condition, and communicated clearly with other team members. It also helps prove that patients were informed of their condition and treatment plan.
Strong documentation practices reduce the risk of litigation or complaints and help resolve claims quickly when they do arise. Providers and institutions should aim to exceed the minimum documentation standards rather than simply meeting them.
A comprehensive wound assessment should contain more than a wound description. It must tell the story of the wound’s progression and how decisions were made over time. Strong documentation practices include:
This list is not comprehensive. The provider should also document the rationale behind each change in treatment plan, especially if deviating from standard protocols. This level of detail helps support clinical decisions if they’re later questioned.
When wound care is delivered outside a clinical environment, such as in patients’ homes, liability considerations become even more complex. Providers may have to adapt to space limitations, variable lighting, or limited access to diagnostic tools. These challenges must be accounted for in both the documentation process and the provider’s insurance coverage.
Policies may need to specify:
We address these factors by maintaining consistent protocols across care settings, ensuring that mobile documentation standards match the quality expected in a clinical environment. As a result, this helps maintain reliability no matter the wound care environment.
Similarly, in any clinical environment, adverse events or near misses must be documented accurately and completely. Incident reporting is not just a risk management tool—it can serve as crucial evidence of a provider’s timely response and willingness to follow institutional protocols. Documentation related to incidents should include:
Professional liability insurers often review these reports in the event of a claim. Therefore, a timely and well-written report can provide context and demonstrate that the provider met professional standards even under challenging circumstances.
Wound care professionals must practice within their licensed scope and receive proper credentialing from their employer or institution. Documentation policies should align with these professional boundaries, and liability coverage should reflect them as well.
For example:
Staying within the appropriate clinical scope protects both the provider and the organization. Liability policies may not cover activities performed outside a provider’s credentials.
What Institutions Can Do to Support Safer Documentation
Medical professionals can take specific steps to reduce liability risks tied to documentation:
Facilities should also make sure their liability coverage includes all relevant care settings, including mobile units and telehealth services.
At West Coast Wound Care, we understand the connection between precise wound documentation and legal protection. Our providers are trained to document assessments clearly, consistently, and in accordance with best practices—whether in a clinic or during a mobile home visit.
To that end, we use structured protocols to ensure that every patient’s record supports continuity of care, communicates effectively with all members of the care team, and helps reduce exposure to risk. This commitment to thorough documentation isn’t just about policies—it’s about delivering safe, accountable wound care across every setting we serve.
Risk management plays a pivotal role in maintaining quality, consistency, and safety in wound care. As mobile and outpatient care continues to evolve, providers are under increasing pressure to meet rigorous clinical documentation standards while mitigating risks tied to patient outcomes, infection control, and regulatory compliance. Proper wound assessment documentation is essential not only for guiding treatment decisions but also for supporting quality assurance and minimizing liability.
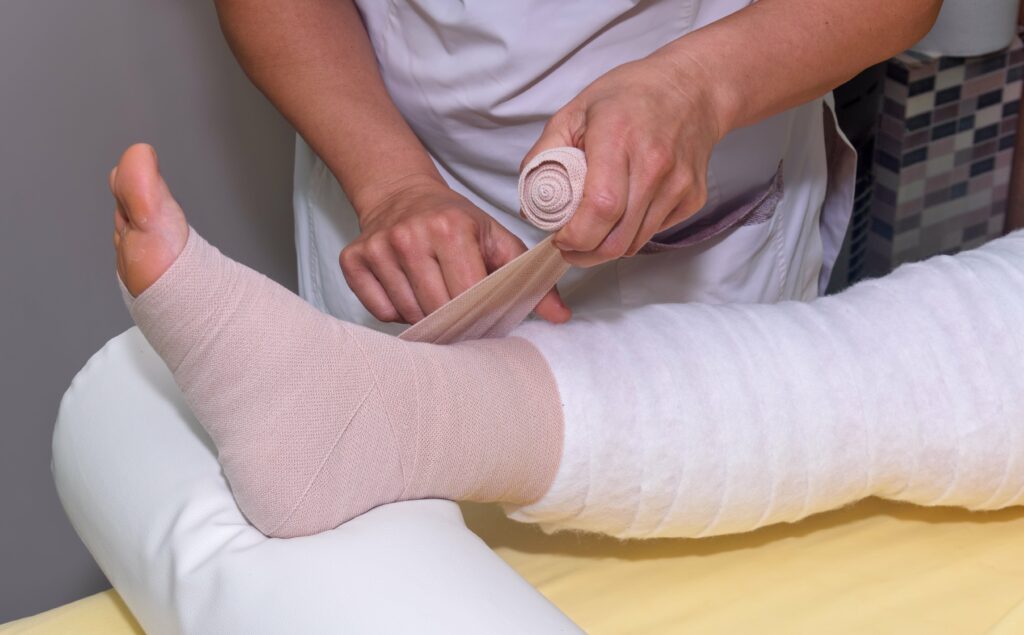
Wound Care and Risk Management
Wound care carries a unique set of challenges compared to many other clinical specialties. Patients often present with multiple comorbidities, delayed healing, or complex surgical wounds, and their recovery can be influenced by social and environmental factors outside the clinic’s control. Each missed or vague entry in a wound record could potentially translate into complications, miscommunication, or delayed interventions.
Risk management in this context extends beyond preventing medical errors. It includes proactively designing processes to ensure accurate documentation, streamline communication across care teams, and comply with regulations from federal and state agencies.
The foundation of strong documentation lies in its clarity, consistency, and comprehensiveness. Each of these qualities can serve as a risk prevention mechanism.
Each missed or vague entry in a wound record could potentially translate into complications, miscommunication, or delayed interventions, which directly impacts safety in wound care.
One of the most common sources of documentation-related risk is inconsistent terminology. For example, a wound described as “large” or “irregular” can be interpreted differently by different clinicians. T
The National Pressure Injury Advisory Panel (NPIAP) and other industry organizations recommend using uniform language to describe wound type, size, depth, exudate, odor, color, and tissue involvement. Departments should create or adopt structured templates that require:
This structured language ensures that care decisions are based on consistent data points, reducing variability and risk across visits.
Transitioning from paper-based to electronic wound assessment tools can greatly reduce documentation errors. Digital platforms that include built-in prompts, checklists, and alerts can catch omissions in real time. Many software platforms now offer secure photo uploads, auto-measurements, and audit trails, adding an extra layer of documentation accuracy.
In mobile wound care, smart tools help staff working independently capture all critical data right at the point of care.
Document the Decision-Making Process, Not Just the Wound
Risk management isn’t just about recording what is seen—it also involves recording why certain decisions are made. For example, if a provider chooses a particular dressing over another or delays debridement due to a patient’s comorbid condition, that rationale should be documented clearly.
This step can serve as protection if there is ever a need to justify treatment decisions during a review or audit. Good documentation helps draw a direct line between clinical observations and the provider’s medical judgment.
The dynamic nature of wound healing means that even a single lapse in updated documentation can compromise care continuity. Inconsistent reassessments can also expose a department to regulatory scrutiny or negative patient outcomes.
Risk management protocols should include scheduled documentation checkpoints, especially for patients with high-risk or non-healing wounds.
Each reassessment should clearly indicate whether the wound has improved, remained stable, or worsened, and include updated images when appropriate.
Wounds don’t always operate in isolation. If a patient with a chronic ulcer develops systemic signs of infection, the documentation should reflect the relationship between wound changes and larger health issues. Including notes on fever, malaise, new drainage odor, or surrounding cellulitis can signal a clinician’s attention to complications such as sepsis or osteomyelitis.
As the Agency for Healthcare Research and Quality (AHRQ) highlights, early recognition and response to systemic risks is a key component of patient safety protocols in wound care.
Including notes on fever, malaise, new drainage odor, or surrounding cellulitis can signal a clinician’s attention to complications such as sepsis or osteomyelitis and improve safety in wound care.
Wound care documentation often focuses solely on clinical findings, but patient and caregiver feedback should be incorporated regularly. If patients report worsening symptoms or caregivers struggle with dressings, those insights help guide needed changes to the care plan.
Ignoring these reports can lead to preventable complications and liability risks. Including subjective observations reinforces a holistic approach to care and reflects patient-centered decision-making.
Risk strategies work best when documentation is seen as a tool for improvement—not just a burdensome administrative requirement. Chart reviews and audits should highlight gaps and also help coach clinicians to improve clarity and reduce inconsistencies in notes.
Treating documentation as a clinical skill—not just a task—improves compliance, morale, and leads to better outcomes for all patients.
Adapt Documentation for Remote or In-Home Care Environments
Mobile care services introduce a unique set of documentation challenges. Lighting, space constraints, and lack of connectivity can interfere with accurate entries. To manage this risk, departments should implement backup methods for documentation when digital systems are unavailable.
Photo documentation protocols must comply with HIPAA and should be stored securely. Clinicians working in the field should also be trained to document environmental factors that could affect wound healing, such as home hygiene conditions or limited access to care supplies.
A well-designed documentation system will include prompts or sections dedicated to reporting incidents, suspected infections, or treatment deviations. Risk managers should regularly analyze these records to identify trends and areas for improvement. These reports don’t just help prevent future problems—they also serve as proof that the department is actively engaged in quality control and patient safety.
Risk increases when documentation fails to support medical necessity for treatments or durable medical equipment. To minimize denials or delays in reimbursement, documentation must align with the clinical criteria required by insurers. This may include documenting failed conservative treatments, measuring wound progress over time, or specifying the goals of care. Inadequate or vague records may trigger audits or payment disputes, which can affect department operations and patient access.
Here, we understand the complexity of wound care documentation and the risks that come with it. By offering both mobile and in-clinic care, we work with providers across a range of settings to ensure continuity and consistency in care.
Our clinical team is trained in industry-standard documentation practices that support accurate assessments, promote effective interventions, and minimize risk for both patients and providers.
We believe that excellent treatment is built on a foundation of detailed, reliable documentation that goes beyond checking boxes. Our goal is to help each patient experience safer healing and better outcomes through informed, collaborative care.
Whether you visit one of our clinics or receive services through our mobile care program, we are committed to supporting every aspect of your healing journey—including the critical documentation that supports it. Schedule an appointment today.
As the landscape of healthcare evolves—with rising patient complexity, longer healing times, and diverse care environments—facilities must update their policies to reflect best practices in wound assessment documentation. These policies are not merely clerical guidelines; they shape clinical outcomes, support compliance, and safeguard patient safety. There are many ways that health care institutions can strengthen their internal policies around wound care documentation. Improved protocols can lead to more consistent, safer, and ultimately more effective patient experiences.
It wouldn’t be an exaggeration to say that at the center of every wound care program is the documentation framework. If hospital policies are unclear, inconsistent, or outdated, care can become fragmented. Inconsistent documentation can lead to missed changes in a wound’s condition, delayed interventions, and poor communication among staff.
Strong institutional policies offer guidance that transcends individual provider preference or experience level.
The policy infrastructure must support clinical, legal, and administrative needs while adapting to new data and standards. When documentation policy is treated as a flexible clinical asset, rather than a static requirement, it enhances care at every level—from bedside practice to leadership review.
Documentation protocols for wound care should:
Developing policies that accomplish all of these goals requires deliberate planning. It also involves a multidisciplinary approach, with input from care providers, nurses, infection control experts, risk management professionals, and compliance officers.
Care often spans hospital rooms, outpatient clinics, long-term care facilities, and patient homes. Inconsistent policies between settings can create information gaps. Therefore, facilities must write documentation policies that address the challenges unique to each location.
For example, hospitals typically rely on electronic medical records with access to a full range of diagnostics and imaging. In contrast, mobile wound care providers working in a patient’s home may face limited resources or need to work offline temporarily.
A one-size-fits-all documentation policy may not be realistic—but alignment across policies should be the goal. Each policy should include minimum standards that apply across settings, then include site-specific addendums.
Documentation policies must be detailed enough to direct provider behavior, yet adaptable enough to handle individual patient needs. The following categories are critical in developing a documentation policy that aligns with clinical excellence and risk mitigation.
Policies should clearly state how often wound assessments must be completed. These timeframes may vary based on wound type, severity, and care setting. Acute surgical wounds may be assessed once per shift in a hospital, while stable chronic ulcers in outpatient care might require documentation every 7 days.
Policies should also outline specific triggers for additional assessments. These could include:
To promote consistency and evidence-based care, institutions should mandate the use of standardized tools. The Bates-Jensen Wound Assessment Tool (BWAT) and the PUSH (Pressure Ulcer Scale for Healing) Tool are commonly used and peer-reviewed. Mandating such tools within policy ensures a structured approach to wound measurement, allowing for trend tracking and treatment efficacy evaluations.
Visual documentation improves diagnostic accuracy and helps demonstrate changes over time. Hospital policies should clarify:
Staff training is critical to making this component reliable. In mobile treatment, clinicians may rely on secure applications that upload photos directly to the patient’s file, allowing for real-time collaboration between field and facility staff.
Many facilities overemphasize checklist documentation and neglect the importance of narrative context. While templates and drop-downs are helpful, hospital policy should ensure that clinicians supplement these tools with narrative entries that capture:
Narratives provide a window into the provider’s clinical reasoning and offer protection in legal or regulatory situations. They also personalize the care record in a way no template can replicate.
Policy should specify how documentation should evolve when wounds do not heal within expected timeframes. Non-healing wounds often require referrals, changes in treatment, or additional diagnostic workup. Documentation should include:
A structured review process may also be built into the documentation policy, so non-healing wounds are automatically flagged for team review after a set number of days.
Wound documentation also plays a role in infection control. The Centers for Disease Control and Prevention (CDC) stresses the importance of infection surveillance in wound care. Proper documentation enables tracking of infection trends and early detection of outbreaks, especially in hospital and post-acute settings. According to the CDC, effective infection prevention depends on timely identification and consistent reporting of wound-related infections (source).
Documentation policy should ensure:
Effective care often involves multiple disciplines: nurses, physicians, physical therapists, dietitians, and case managers. Good policy facilitates communication between these roles. Documentation protocols should support this interdisciplinary model by requiring:
Such documentation improves care continuity, enhances decision-making, and reduces the risk of redundant or conflicting interventions.
Policies alone do not ensure compliance—education must follow. Hospitals and outpatient programs should provide training that reinforces documentation policy, addresses areas of common error, and introduces any updates. Simulation labs, peer reviews, and competency checks can reinforce policy adherence in both new hires and experienced staff.
Regular audits should review documentation for consistency with policy, identifying areas that require policy revision or further training. A strong feedback loop makes policy implementation more dynamic and responsive.
West Coast Wound Care: Here to Help
Hospitals and outpatient settings face ever-growing demands to deliver effective care while adhering to evidence-based protocols.
At West Coast Wound Care, we understand that exceptional care relies on clear documentation and the policies that shape it. Whether serving patients at one of our clinics or providing care in the comfort of their homes, we follow structured documentation approaches that reflect industry best practices and regulatory expectations.
We prioritize consistency, transparency, and collaboration across care settings. Our team works with the latest tools and up-to-date standards to make sure each wound assessment tells a clear and complete clinical story. This focus on documentation doesn’t just meet compliance goals—it supports safer, smarter care that truly centers the patient.
If you’re looking for a provider that understands the connection between sound documentation policy and clinical excellence, West Coast Wound Care is here to help.
In the field of wound care, the way we document assessments is just as critical as the treatments we provide. When we take care of patients with complex wounds—including diabetic ulcers, pressure injuries, and trauma-related wounds—every detail we record in the wound care assessment helps guide treatment, protect patients, and maintain regulatory compliance.

At West Coast Wound Care, we emphasize a documentation process that supports precision, communication, and continuity in all the care we deliver.
We don’t treat wounds in isolation. We treat the whole patient. That’s why documentation goes beyond charting wound size or appearance. Our clinical notes must reflect the full picture, from comorbidities affecting healing to the patient’s functional limitations and risk factors. Documentation supports:
By accurately tracking a wound’s progression over time, we can ensure patients receive interventions that are timely, medically necessary, and tailored to their needs.
At West Coast Wound Care, we use structured documentation formats to ensure consistency across different clinicians and care sites. Every wound care assessment we perform is built around clear categories that capture clinical, visual, and patient-reported data.
Each patient record includes:
This structure is essential when patients receive both mobile and clinic-based care. With this level of consistency, all members of the team can quickly interpret notes and follow up accordingly.
We know that incomplete or vague documentation can disrupt care. Even small omissions in a wound care assessment note can result in delayed treatments, billing issues, or substandard care continuity.
That’s why we focus on quality documentation training and regular internal reviews. By reviewing sample entries and holding team discussions, we identify where greater clarity or specificity is needed.
For example, describing a wound as “healing” without measurements or visual indicators leaves too much open to interpretation. I
Instead, we document: “Wound dimensions decreased from 3.0 cm x 2.5 cm x 0.5 cm to 2.4 cm x 2.1 cm x 0.2 cm over seven days; increased granulation tissue present, with no signs of infection.” That kind of clarity makes a difference in how the care plan is shaped.
Regulatory agencies use our documentation to assess the quality of our wound care delivery. In long-term care settings, for example, pressure injury data collected through assessments feeds directly into quality metrics tracked by the Centers for Medicare & Medicaid Services (CMS). These data points can influence public facility ratings and impact reimbursement.
That’s why we take particular care when staging pressure injuries and documenting their progression. We follow guidance from CMS and national panels such as the National Pressure Injury Advisory Panel (NPIAP), making sure we reflect the latest classification definitions.
CMS’s Resource Utilization Group (RUG) scores and Minimum Data Set (MDS) assessments rely on this information to determine care complexity and associated reimbursement. As outlined in the CMS RAI Manual, pressure injury reporting is more than a formality—it has direct financial and care delivery implications.
Another layer we consider in documentation is patient engagement. Our mobile care providers often meet patients in their homes, where they can get a clearer sense of how living conditions, lifestyle, and caregiver support affect wound healing. We integrate those findings into our notes so they can inform decisions about dressing types, follow-up frequency, and self-care education.
By documenting what we observe in real-time, we provide better support for individualized treatment. For instance, a patient who lives alone and has arthritis may need simpler dressing regimens than a patient with a full-time caregiver. Including that context ensures care plans are realistic and actionable.
We often treat patients with wounds that don’t fall neatly into a single category. Radiation injuries, mixed arterial-venous ulcers, and wounds complicated by autoimmune conditions all require a higher degree of documentation precision.
In these cases, we ensure our notes include:
We also incorporate wound photographs when appropriate, securely storing them as part of the patient record. This helps track subtle changes in color, size, or infection risk, especially when comparing assessments from multiple clinicians.
Patients often move between settings—hospital, clinic, and home. We design our documentation so that any provider, with access to the wound care assessment, can quickly understand the wound’s current condition and treatment history.
This is especially important in discharge summaries, which must include wound status, outstanding needs, and instructions for continued care. When patients receive services across locations, we ensure our notes help eliminate duplication, reduce delays, and avoid treatment gaps.
We view documentation as a clinical skill that requires ongoing training. West Coast Wound Care regularly updates our team on changes in documentation expectations from regulatory and professional organizations.
This process helps clinicians:
Our clinical leadership team encourages a culture where asking questions about documentation best practices is welcomed. We believe continuous learning improves both patient outcomes and compliance.
As regulations and science evolve, so do expectations for documentation. West Coast Wound Care tracks new developments in:
By adapting our practices and updating internal protocols, we help ensure that our documentation not only meets current standards but anticipates future changes.
Connecting Good Documentation to Patient Outcomes
When documentation is accurate, comprehensive, and timely, our patients benefit. They receive better-coordinated care, faster interventions when complications arise, and fewer disruptions due to billing or regulatory issues. Our team can spot patterns more quickly and adjust plans based on real data rather than assumptions.
At West Coast Wound Care, our commitment to documentation excellence is part of our larger mission to deliver high-quality, individualized wound care in the settings most convenient for our patients—whether at home or in one of our clinics. We treat documentation not just as a task, but as a clinical tool that drives outcomes, transparency, and trust.
To see how we can help you and yours, schedule an appointment.
Infection control and preventing infection are some of the most important wound care services that we provide. Always, we follow OSHA (the Occupational Safety and Health Administration) regulations when doing so. These protect both healthcare providers and patients by mandating safe practices in medical environments.
These regulations can serve as part of the foundation for infection prevention protocols across healthcare settings. At West Coast Wound Care, we follow OSHA regulations closely to maintain safe, hygienic environments wherever care is delivered, incorporating these standards into our patient-centered services.
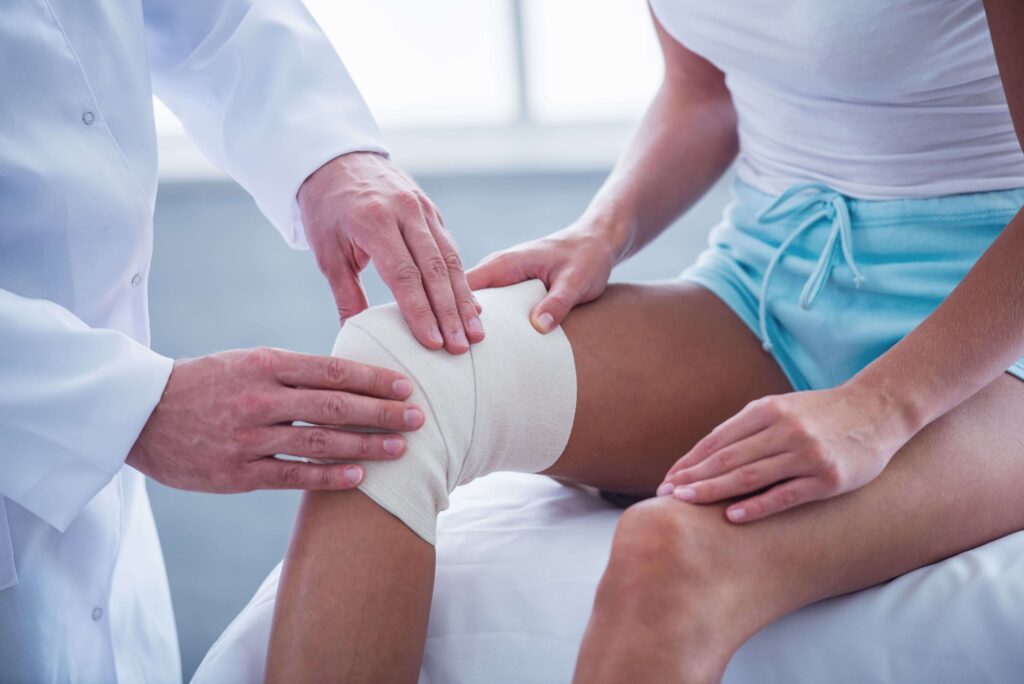
Open wounds, especially those that are deep, draining, or slow to heal, unfortunately, create opportunities for microbial entry. When combined with underlying conditions like diabetes or compromised circulation, wounds can quickly become infected if protocols aren’t followed.
OSHA’s regulations are not optional—they are mandatory for all healthcare employers, including us. These regulations are designed to:
Because we work in patients’ homes, long-term care facilities, and dedicated clinics, these regulations help us maintain consistent infection control standards wherever we provide care.
The most applicable OSHA rule to wound care is the Bloodborne Pathogens Standard (29 CFR 1910.1030). This regulation requires healthcare employers like us to implement practices that reduce occupational exposure to blood and other potentially infectious materials (OPIM). Since wound care often involves direct contact with bodily fluids, complying with this standard is essential.
Key OSHA-mandated infection control practices include:
All these practices are part of our services and help reduce infection risks. (OSHA Bloodborne Pathogens Standard – OSHA.gov)
While the Bloodborne Pathogens Standard remains central, several recent developments have deepened the importance of infection control:
These shifts underscore the need for infection prevention strategies tailored to every patient, whether at a clinic or in the field.
We’ve embedded OSHA compliance into everything we do at West Coast Wound Care. Whether we’re seeing a patient in one of our clinics or visiting them at home, we follow the same rigorous safety standards.
Here’s how we do it:
By keeping these systems in place, we protect both our patients and our staff while delivering high-quality care.
We specialize in providing a wide range of wound care services, and we do so in a way that prioritizes safety, infection prevention, and patient comfort. Our care team is trained to treat:
Our treatments include:
Everything we do is supported by documentation and safety protocols that meet OSHA standards, ensuring continuity and excellence in care.
If you or someone you know is in need of reliable, skilled, and infection-conscious care—delivered either in a clinic or right at home—we’re ready to help. At West Coast Wound Care, we combine safety with compassion to help wounds heal the right way. Reach out for more information or to schedule an appointment to see how we can treat infection and more.
When you leave a hospital, you, rightfully, might assume your recovery is on the right track. Hospitals play a critical role in healthcare. They can do so much for the wounded. They can provide urgent treatment that prevents wounds from worsening. However, for many patients, complete healing is a longer and more complex process than hospitals are equipped to handle. That’s where specialized wound care, like what we offer, can make the difference.
If you or a loved one has been discharged from a hospital but still requires care, understanding the next steps in your recovery is crucial.
For patients with wounds, whether from surgeries, injuries, or chronic conditions, hospitals focus on stabilizing the area to prevent complications. They’ll clean and dress wounds, manage infections, and address symptoms like pain or swelling. While hospitals are excellent at providing immediate treatment and preventing further damage, they often fall short in delivering long-term wound healing.
Why? Healing a wound completely requires ongoing, specialized care that hospitals are neither designed nor staffed to provide.
For example, chronic wounds such as certain ulcers, need specialized treatments that go beyond basic care. These might include advanced dressing techniques, nutritional guidance, infection management, or regular monitoring of the affected area.
Hospitals typically discharge patients once their condition no longer requires inpatient care, even if their wounds haven’t fully healed.
This disconnect can leave many patients vulnerable, unsure of how to proceed with the necessary care at home or in another setting.
Wounds that aren’t appropriately cared for after a hospital stay can lead to complications. Wounds aren’t on a schedule. They don’t follow a chart.
Withoutmonitoring and treatment, issues like infection, tissue damage, or delayed healing can arise. This is especially true for individuals managing chronic conditions like diabetes or vascular disease. Wounds may worsen rapidly without the proper expertise and attention, which can cause additional hospital readmissions or, in severe cases, life-altering consequences such as amputation.
For many patients, follow-up wound care is essential to ensure proper healing. However, navigating the options for care after being discharged can be overwhelming. Skilled nursing facilities (SNFs) and home health teams play a role by providing basic wound maintenance and comfort. Still, many patients need treatment options that go beyond the traditional care services.
This is where we step in to bridge the gap. Our team of skilled technicians provides personalized, advanced treatment to help patients recover fully.
One of the ways we can help is to provide treatment in your home. Depending on your location, we can provide mobile care. This means our team comes directly to patients, whether they’re in a skilled nursing facility or recovering in their own homes. This personalized approach not only makes care more accessible but also ensures that the specific needs of each wound are addressed consistently and professionally.
Advanced Techniques for Recovery
Healing a wound takes more than just cleaning and bandaging. We use cutting-edge treatment methods tailored to each patient. Our team specializes in addressing chronic wounds, infections, and underlying conditions that may hinder the recovery process.
Comprehensive Skin Sweeps
For patients in skilled nursing facilities, one of our more popular offerings is our detailed skin sweeps. Among the many benefits, these can help identify potential wound care issues early, preventing minor skin problems from escalating. This can significantly improve healing outcomes.
Preventing Hospital Readmissions
Providing specialized wound care at home or in a SNF not only speeds up recovery but also reduces the risk of complications that might require another hospital stay. Through this, we can give patients peace of mind, knowing that their wounds are healing correctly under expert supervision.
Holistic Approach to Care
Our care isn’t just about the physical wound itself. West Coast Wound Care adopts a holistic approach, addressing contributing factors like nutrition, infection risks, and patient education. By focusing on the whole picture, they set patients up for sustainable healing.
We work closely with skilled nursing facilities to enhance wound treatment programs. While SNFs are excellent at providing general care and comfort, many lack the specialized knowledge and resources needed to heal complex wounds fully. By partnering with SNFs, we can bring our care directly to these facilities, offering advanced interventions tailored to each patient’s needs.
Their collaborative relationships with SNFs mean better outcomes for patients and peace of mind for their families. Staff and loved ones can trust that we’ll track, monitor, and adjust treatment plans to ensure optimal healing.
If you’ve recently been discharged from a hospital and still need care, there’s plenty you can expect when working with West Coast Wound Care.
Our team carefully examines your wound, overall health, and any underlying conditions to develop a customized treatment plan.
Instead of visiting multiple hospitals and so forth, our techs can bring care directly to you, whether you’re at home or in a SNF.
Healing can be a lengthy process, but West Coast Wound Care offers regular check-ins and adjustments to treatment as needed.
Whether working with hospital discharge teams, SNF staff, or primary care providers, we can ensure a seamless transition and consistent communication to support your care.
At the end of the day, proper care is about more than avoiding complications; it’s about regaining your health, mobility, and confidence. Despite their best efforts, traditional care settings like hospitals and SNFs often aren’t equipped to support complete healing. That’s exactly why West Coast Wound Care exists—to offer specialized services that guide patients through the critical phases of recovery.
If you or a loved one has been discharged from a hospital and has wounds that need continued care, we’re here to help.
Continue the healing process today. Your recovery matters. Reach out now to schedule an appointment and see how we can help.
You’re Discharged From a Hospital and Still Need Wound Care. What to do?
Wound healing is a process that, unfortunately, many people unknowingly sabotage by making common mistakes. Whether it’s a minor cut or a more complex chronic wound, improper care can worsen the situation, prolong healing, and even lead to severe complications. Understanding what is the wound healing function and avoiding common errors can make all the difference in achieving a faster, healthier recovery.
At West Coast Wound Center, we specialize in providing accessible and personalized care for wounds of all types. By addressing the whole person and offering state-of-the-art treatments, we empower patients to heal properly.
Here’s what you need to know about how wounds heal, what you might be doing wrong, and how we can help.
When caring for a wound, even well-intentioned actions can sometimes cause more harm than good. Here are some of the most frequent missteps that hinder the healing process.
Failing to clean a wound properly is one of the most common mistakes. Dirt, bacteria, and debris left in the wound can lead to delayed healing or even infection. While it might be tempting to rinse it quickly and move on, proper cleaning with a gentle antiseptic solution is necessary to prevent complications. That, obviously, won’t fully heal a wide range of wounds. But, it’s an important early, initial step.
Peeking under a dressing to check how a wound is healing disrupts the environment necessary for recovery. Wounds heal best in a moist and covered setting. Removing the dressing prematurely can expose the wound to bacteria and delay progress.
Antibiotic ointments can be helpful, but overuse may irritate the wound or cause further skin issues. Some individuals also apply heavy creams indiscriminately, which can block oxygen flow, critical for healing.
Sometimes, people underestimate the severity of their wounds. Not seeking professional medical care leads to untreated infections, chronic wounds, or complications like cellulitis or sepsis.
Activities that irritate the wound, such as scratching or failing to rest an injured body part, prolong healing time. Even small repetitive injuries to the area can prevent repair.
Underlying conditions like diabetes, poor circulation, or a weakened immune system can delay or even prevent healing. Failing to manage blood sugars, for instance, can result in non-healing diabetic ulcers.
Now that we’ve identified these common pitfalls, it’s important to understand how wounds actually heal and what steps you can take to support that natural process.
The human body has an incredible ability to repair itself, but wound healing function involves a complex series of steps. Here’s a breakdown of how it works.
This is the immediate response to a wound. Your body forms a clot to stop the bleeding and create a barrier against bacteria. This clot consists of platelets and fibrin, which kickstart the healing process.
Once the wound is sealed, your body activates immune cells to clean out bacteria and debris. This is why wounds often appear red, warm, and slightly swollen during the first days. While inflammation is part of the process, excessive inflammation can signal infection.
Now, your body begins to create new tissue to repair the damage. Fibroblasts produce collagen to close the wound, and new blood vessels form to deliver oxygen and nutrients. This phase is essential for rebuilding strength in the affected tissue.
Finally, your body strengthens the newly formed tissue by reorganizing the collagen. While this phase can last weeks for small wounds, larger or chronic wounds may take much longer to fully heal, resulting in scars.
At West Coast Wound Center, we understand that each wound is unique. Our comprehensive approach focuses on the entire person, not just the injury, to provide tailored solutions for optimal healing. Here’s how we can support you.
We offer advanced, evidence-based treatments designed to promote faster and more effective recovery. Some of our services include surgical debridement to remove damaged tissue, compression therapy for conditions like venous ulcers, and skin grafting for severe injuries or burns.
No two wounds are the same, and our specialists understand that healing requires a personalized approach. We consider not only the wound itself but also underlying factors such as medical history, nutrition, and circulation to design a care plan just for you.
Many of our patients struggle with chronic wounds resulting from conditions like diabetes, pressure sores, or venous insufficiency. Our expertise in managing complex wounds ensures that you receive the specialized care your condition requires.
Our team uses state-of-the-art technology to assess and treat wounds. From cryotherapy to reduce inflammation and promote faster healing to telemedicine options for follow-up care, we integrate innovation into everything we do.
We don’t just treat your wounds; we help you avoid future complications. Our team educates patients on proper wound care techniques, lifestyle adjustments, and strategies for managing underlying health conditions.
With both mobile services and clinic locations, we make wound care accessible and convenient. Whether you need a home visit or can visit us in Fresno, Northridge, or Inglewood, we ensure you get the care you deserve without unnecessary hassle.
By focusing on proper care, avoiding preventable mistakes, and working with experienced wound care specialists, you can significantly improve your healing outcomes.
West Coast Wound Center is here to guide you every step of the way. Don’t wait for wounds to worsen or become unmanageable. Contact us today to book an appointment and take another step of healing.