For many patients, especially older adults, the idea of surgery can feel overwhelming. Fortunately, modern medicine offers effective alternatives that avoid traditional surgical environments. Our approach to wound care focuses on safe, targeted treatment that can often be performed outside the operating room.
Through bedside procedures, advanced technologies, and coordinated care, we help patients receive treatment in familiar surroundings while reducing the risks commonly associated with hospital-based procedures.
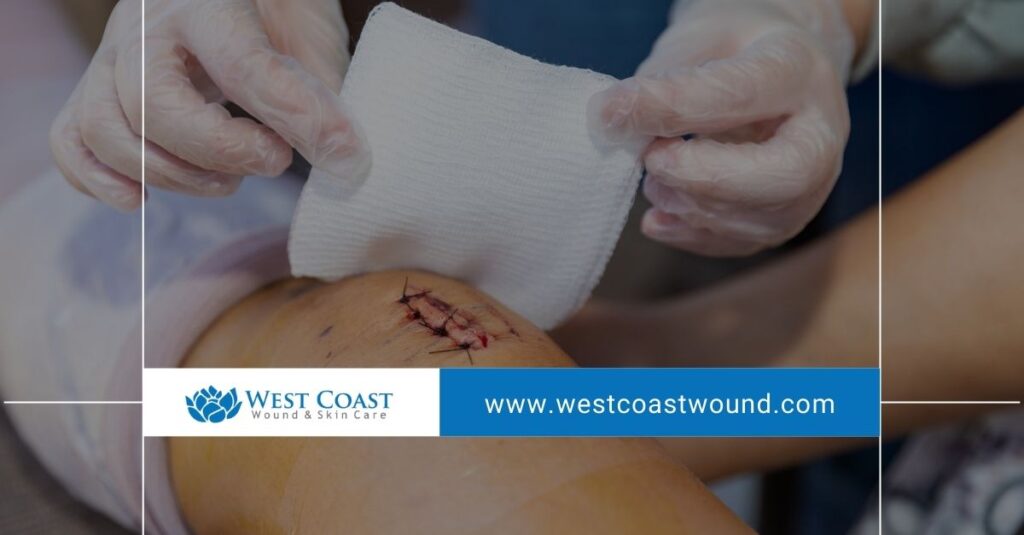
How Debridement Helps Chronic Wounds Heal
Removing Tissue That Prevents Recovery
Debridement is a medical procedure used to remove dead, damaged, or infected tissue from a wound. This tissue, often referred to as necrotic material, creates an environment where bacteria thrive and healing slows down. In addition to necrotic tissue, chronic wounds frequently develop biofilm—a layer of microorganisms that protects bacteria from treatments.
When these materials accumulate, the body struggles to rebuild healthy tissue. Debridement clears away these barriers so the natural healing process can begin again.
Healthcare research consistently shows that removing unhealthy tissue can transform a stagnant wound into one that actively heals. This process is sometimes described as resetting the wound’s healing timeline.
Patients who receive professional wound care often see improved outcomes once the wound bed is properly prepared for healing.
Precision Treatment at the Bedside
Our wound care specialist team performs sharp debridement using sterile instruments designed to remove unhealthy tissue with precision. These tools are similar to those used in surgical settings but are applied in a controlled, bedside environment.
This approach allows us to remove only damaged material while protecting surrounding healthy skin. By targeting the specific areas that require treatment, we can often help wounds progress toward healing without the need for an operating room.
For many patients, this option makes wound care more accessible and less intimidating.
Why Hospital-Based Procedures Are Not Always Necessary
Reduced Risks Related to Anesthesia
General anesthesia is a necessary component of many surgical procedures, but it carries risks for certain individuals. Seniors and patients with heart conditions, respiratory issues, or other chronic illnesses may face complications when undergoing anesthesia.
Bedside procedures typically rely on local numbing methods instead. Patients remain awake during treatment while the targeted area is safely desensitized.
Benefits of local anesthesia may include:
- Reduced cardiovascular stress
- Faster recovery time
- Lower likelihood of medication complications
By performing targeted treatments outside the operating room, we can help reduce these risks while still providing effective care.
Avoiding Facility-Acquired Infections
Hospitals provide essential medical services, but they also expose patients to environments where bacteria circulate among large numbers of individuals. Certain strains of bacteria, including drug-resistant organisms, are more commonly found in healthcare facilities.
Receiving treatment through mobile services or at our advanced wound care centers can help reduce exposure to these pathogens.
Lower exposure to facility-acquired infections is particularly valuable for individuals with weakened immune systems or chronic wounds that already face healing challenges.
Reducing Physical and Emotional Stress
Hospital procedures can require extensive preparation, transportation, and recovery time. For patients living in assisted living facilities or recovering from illness at home, traveling to a surgical center may involve ambulance transport, long waiting periods, and significant fatigue.
By offering bedside procedures and mobile visits, we remove many of these logistical barriers. Patients can receive treatment without leaving the environment where they already feel comfortable and supported.
Modern Debridement Technology at the Bedside
Ultrasonic Debridement Techniques
Advances in wound treatment technology have expanded the options available outside traditional surgical suites. Ultrasonic debridement is one example of these innovations. Studies have shown it can be very effective.
This technique uses low-frequency ultrasound waves to break apart bacteria, debris, and biofilm that collect within chronic wounds. The vibrations help separate unhealthy material from healthy tissue.
Potential benefits include:
- Reduced trauma to surrounding skin
- Minimal bleeding during treatment
- Efficient removal of bacterial buildup
Because the technology targets unwanted material selectively, it supports faster wound bed preparation and healing progression.
MIST Therapy for Post-Debridement Recovery
After unhealthy tissue is removed, the wound environment must be carefully managed to encourage new tissue growth. One technology used for this purpose is MIST Therapy.
This treatment delivers low-frequency ultrasound energy through a saline mist. The gentle energy stimulates cellular activity within the wound while avoiding direct contact with the sensitive area.
MIST Therapy may help:
- Promote cellular regeneration
- Improve circulation in the wound bed
- Reduce bacterial presence
These treatments can be incorporated into ongoing care plans that support long-term healing.
Preventing Pressure Injuries Before They Develop
Debridement plays a key role in treating wounds, but prevention remains the most effective strategy. Patients who spend extended periods in bed or seated positions face increased risk of developing pressure injuries.
These injuries form when continuous pressure reduces blood flow to certain areas of the body. Without adequate circulation, tissue begins to deteriorate.
Repositioning to Protect Skin Health
One of the most effective prevention strategies is regular repositioning. Shifting body weight allows oxygen and nutrients to return to compressed tissues.
Caregivers often follow repositioning schedules that encourage movement every couple of hours. Even small changes in position can significantly reduce pressure on vulnerable areas.
Helpful practices include:
- Alternating between left and right side positions
- Elevating heels with supportive cushions
- Adjusting seating posture frequently
These measures help maintain circulation and protect delicate skin.
Supportive Surfaces That Reduce Pressure
Specialized mattresses and cushions can distribute body weight more evenly, decreasing pressure on areas where bones press close to the skin.
Support surfaces recommended for at-risk patients may include:
- Advanced foam mattresses
- Pressure redistribution overlays
- Cushioned wheelchair supports
These tools help maintain consistent pressure relief throughout the day and night.
Maintaining Clean and Dry Skin
Moisture can weaken the skin’s protective barrier. Sweat, wound drainage, or incontinence can all contribute to skin breakdown when not managed properly.
Preventive care focuses on:
- Gentle cleansing with skin-friendly products
- Applying protective moisture barriers
- Regularly changing linens and clothing when damp
These practices help maintain skin strength and reduce the likelihood of irritation.
Recognizing Early Signs of Pressure Injuries
Identifying pressure injuries early makes treatment significantly easier. Stage 1 pressure injuries may appear as persistent redness that does not fade when pressure is applied.
Other early indicators include:
- Localized warmth or firmness
- Mild swelling around the area
- Sensitivity or discomfort when touched
Prompt attention to these symptoms allows medical providers to intervene before the skin opens or deeper tissue damage develops.
For patients receiving wound care, early detection plays a critical role in preventing complications.
Nutrition and Skin Resilience
Supporting Tissue Repair Through Diet
Skin is a complex organ that requires proper nutrition to maintain strength and elasticity. Individuals with limited mobility or chronic illness may struggle to obtain the nutrients necessary for tissue repair.
Our approach to holistic wound care includes coordination with dietary professionals who help patients maintain balanced nutrition.
Essential nutrients for skin health often include:
- Protein for building new tissue
- Vitamin C for collagen formation
- Vitamin E for cellular protection
- Zinc for immune support
A balanced diet supports both wound healing and overall wellness.
Hydration and Circulatory Support
Adequate hydration also contributes to healthy skin. Fluids help maintain circulation, allowing oxygen and nutrients to reach tissues more effectively.
Patients who remain properly hydrated may experience improved skin resilience and better healing outcomes.
In certain situations, dermatology care may also support skin health when underlying conditions contribute to fragility or irritation.
Accessible Treatment Through Mobile Services and Clinics
Our providers offer care in multiple settings to ensure patients receive timely treatment. Some individuals benefit from visits to our advanced wound care centers, while others prefer care delivered directly to their homes or care facilities.
Mobile visits allow clinicians to evaluate wounds, perform treatments, and monitor healing without requiring patients to travel.
This flexibility helps ensure that patients receive consistent care regardless of mobility limitations.

Debridement and the Future of Wound Care
Advances in medical technology have transformed how clinicians approach chronic wounds. Many procedures that once required operating rooms can now be safely performed in more comfortable environments using precise tools and modern treatment techniques.
Debridement remains one of the most effective ways to stimulate healing when wounds become stalled. By combining this procedure with advanced therapies, prevention strategies, and personalized treatment plans, we help patients regain progress in their recovery.
Through comprehensive wound care, patients can access modern treatments designed to promote healing while minimizing the risks and disruptions often associated with hospital-based procedures.
