Chronic wounds affect millions of Americans each year, with an estimated 6.5 million people living with wounds that do not close properly. Non-healing wound treatment is possible. Many wounds that seem as if there is no treatment for them genuinely can be treated.
Unlike minor cuts or abrasions, these wounds remain open for weeks or even months, often because the body’s natural repair process has been disrupted.
When left untreated, chronic wounds can lead to serious complications, including infection, ongoing pain, limited mobility, hospitalization, and in severe cases, tissue loss or amputation. Early diagnosis and proper care can make a significant difference.
What Is a Non-Healing Wound?
A non-healing wound, often called a chronic wound, is an injury that does not progress through the normal stages of repair. Healthy skin injuries generally close in a predictable timeframe. Chronic wounds stall in one or more phases of recovery.
The reasons vary from patient to patient, but these wounds are often linked to:
- Reduced blood circulation
- Diabetes or vascular disease
- Repeated pressure or friction
- Infection
- Nutritional deficiencies
- Immune system dysfunction
Because many chronic wounds are connected to underlying medical issues, successful non-healing wound treatment usually addresses more than the surface injury alone.
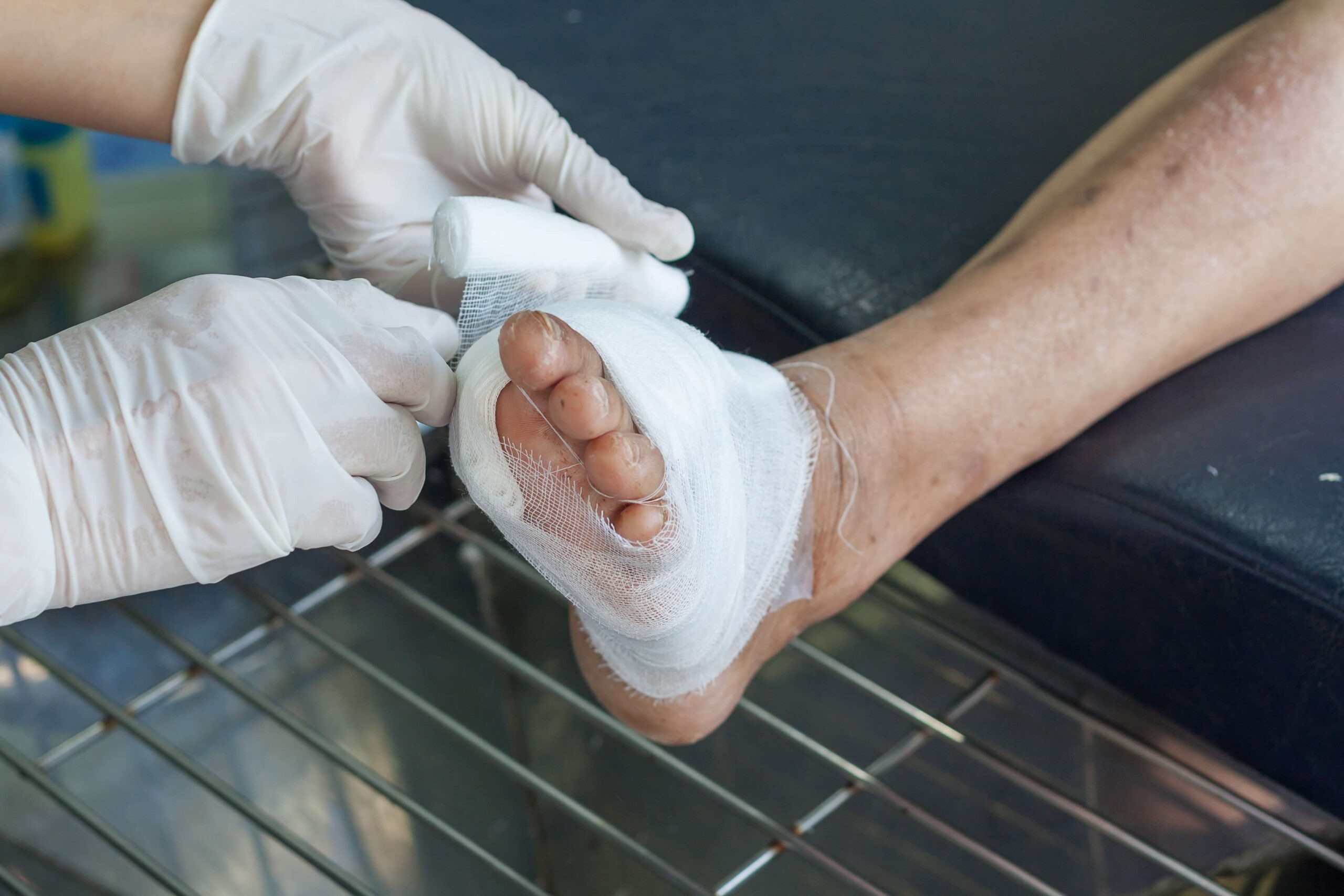
Common Types of Non-Healing Wounds
Pressure Ulcers
Pressure ulcers, sometimes called bedsores, develop when prolonged pressure reduces blood flow to the skin and underlying tissue. They often form on areas such as the heels, hips, tailbone, and elbows.
People who spend extended periods in bed or in a chair are especially vulnerable.
Treatment commonly includes:
- Frequent repositioning
- Pressure-relieving mattresses or cushions
- Moisture management
- Removal of damaged tissue when needed
Without early intervention, pressure ulcers can quickly deepen and become difficult to manage.
Diabetic Ulcers
Diabetic ulcers most often appear on the feet or lower legs. Nerve damage and reduced circulation make them especially dangerous because patients may not notice injuries right away.
Untreated diabetic ulcers may lead to:
- Infection
- Tissue death
- Gangrene
- Hospitalization
Prompt non-healing wound treatment can reduce the risk of serious complications and improve outcomes.
Venous Ulcers
Venous ulcers typically develop near the ankles and lower legs. They occur when veins cannot efficiently return blood to the heart, causing blood to pool in the lower extremities.
Common signs include:
- Swelling
- Skin discoloration
- Aching or heaviness in the legs
- Persistent drainage
Compression-based therapies are often an important part of care for venous wounds.
Arterial Ulcers
Arterial ulcers result from poor blood flow caused by narrowed or blocked arteries. Because oxygen and nutrients cannot adequately reach the tissue, healing becomes difficult.
These wounds are often:
- Painful
- Located on the feet, toes, or lower legs
- Pale, dark, or sharply defined in appearance
Treatment often focuses on improving circulation while protecting the wound from further damage.
Non-Healing Surgical Wounds
Sometimes a surgical incision does not close as expected. This can happen because of infection, poor circulation, repeated irritation, or underlying health conditions.
When a surgical wound remains open, prompt medical assessment is important to prevent deeper complications.
What Causes Chronic Wounds?
Many chronic wounds develop because several factors interfere with normal repair.
Infection
Bacteria can slow recovery by damaging tissue and producing toxins that interfere with cellular repair.
Poor Circulation
Blood delivers oxygen and nutrients essential for tissue repair. Conditions such as diabetes, vascular disease, and hypertension can reduce circulation and delay progress.
Age
As people age, skin becomes thinner and the body’s regenerative ability may slow.
Repeated Trauma
Constant rubbing, pressure, or accidental re-injury can prevent closure.
Medication Effects
Certain medications may interfere with the inflammatory and regenerative processes required for tissue repair.
A wound care specialist team can evaluate these contributing factors and build a treatment strategy based on the patient’s medical history.
Who Is Most at Risk?
Some individuals are more likely to need non-healing wound treatment than others.
Higher-risk groups include people with:
- Diabetes
- Peripheral artery disease
- Venous insufficiency
- Cancer
- Reduced mobility
- Weakened immune systems
- A history of previous ulcers
Lifestyle habits can also increase risk. Smoking, poor nutrition, and inactivity may all negatively affect circulation and tissue repair.
For patients who have difficulty traveling, mobile wound care can make expert treatment more accessible while reducing delays in care.
Warning Signs That Need Medical Attention
A chronic wound often worsens gradually. Early evaluation can prevent more serious complications.
Seek medical attention if you notice:
- Redness that does not improve
- Increasing pain
- Drainage or leakage
- Unpleasant odor
- Swelling around the wound
- Darkened or discolored edges
- Skin breakdown that continues to spread
Recognizing these symptoms early can support faster wound healing and reduce the risk of infection.
Non-Healing Wound Treatment Options
There is no single solution for every chronic wound. Treatment depends on the wound’s type, size, location, and underlying cause.
Debridement
Debridement removes dead or damaged tissue. This helps reduce bacterial burden and encourages healthy tissue growth.
Compression Therapy
Often used for venous ulcers, compression can reduce swelling and support better blood flow in the lower legs.
Nutritional Support
Protein, vitamins, hydration, and overall dietary balance can influence tissue repair. In some patients, nutritional deficiencies significantly slow recovery.
Biopsies
When a wound behaves unusually or fails to respond, a biopsy may help identify hidden causes.
Cryotherapy
Cryotherapy may be used in selected cases to reduce inflammation and assist tissue management.
Medications
Treatment may include:
- Antibiotics for infection
- Topical antimicrobial products
- Prescription ointments based on wound type
Adjunctive Therapies
Advanced treatments such as oxygen therapy or pressure-based therapies may be considered for certain chronic wounds.
In some cases, holistic wound care can also play a valuable role by addressing circulation, nutrition, mobility, skin protection, and long-term prevention alongside direct wound management.
Why Proper Wound Dressings Matter
Dressings are more than simple coverings. The right dressing protects the wound while maintaining an environment that supports tissue repair.
Different wounds may require different dressing types depending on:
- Drainage level
- Infection risk
- Tissue condition
- Wound depth
- Healing stage
Because every wound behaves differently, professional guidance can help determine the most appropriate dressing and replacement schedule.
Personalized Care for Better Recovery
Successful non-healing wound treatment often requires ongoing monitoring and adjustments over time. A wound that looks stable one week may need a different approach the next.
When chronic wounds receive timely attention, patients often experience less pain, improved mobility, and a better overall quality of life.
If a wound has remained open longer than expected, early evaluation can be one of the most important steps toward recovery.
FAQs About Non-Healing Wound Treatment
What is a non-healing wound?
A non-healing wound is an injury that does not close within the expected timeframe, often lasting for weeks or months. These wounds typically stall due to underlying issues such as poor circulation, infection, or chronic conditions like diabetes.
What are the most common types of chronic wounds?
The most common types include pressure ulcers, diabetic ulcers, venous ulcers, arterial ulcers, and non-healing surgical wounds.
Who is at higher risk for developing chronic wounds?
People with diabetes, vascular disease, weakened immune systems, or limited mobility are at greater risk. Lifestyle factors like smoking, poor nutrition, and inactivity can also increase the likelihood of developing wounds that do not heal properly.
What are the warning signs that a wound is not healing correctly?
Signs include persistent redness, increasing pain, swelling, drainage, foul odor, and dark or discolored edges. If any of these symptoms appear, seeking medical care early can help prevent complications and support faster recovery.
What treatments are available for non-healing wounds?
Treatment options vary depending on the wound type and severity. Common methods include debridement, compression therapy, medications, advanced therapies, and proper wound dressings.
