Research has shown that a significant percentage of patients with venous leg ulcers experience healing within six months when compression is applied correctly.
What Is Compression Therapy in Wound Care?
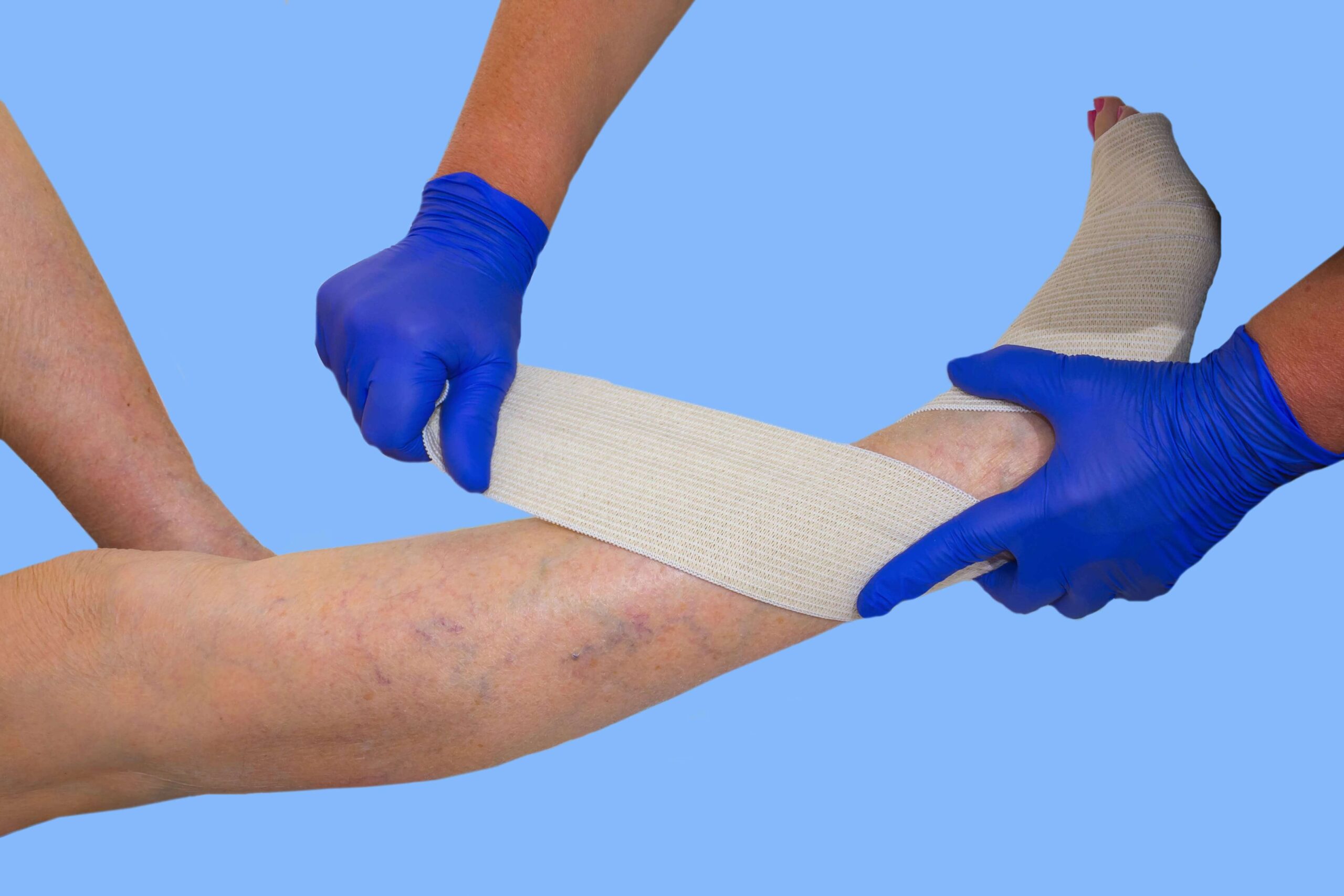
Compression therapy involves the use of specialized bandages, wraps, or garments that apply controlled pressure to the lower extremities. This pressure helps veins function more efficiently by encouraging blood to flow upward toward the heart.
By improving circulation, compression therapy helps:
- Reduce fluid buildup in tissues
- Decrease venous pressure
- Limit swelling and inflammation
- Support overall wound healing
This targeted approach addresses the root causes of many chronic wounds rather than just treating surface symptoms.
How does compression therapy help wounds heal faster?
By applying controlled pressure, compression therapy enhances blood flow to the affected area. This improved circulation delivers more oxygen and nutrients to tissues, which supports faster and more effective wound healing.
Who can benefit from compression therapy?
Individuals with conditions like edema, venous ulcers, deep vein thrombosis (DVT), and poor circulation often benefit from compression therapy. A medical evaluation is necessary to determine if it is appropriate for each patient.
When Is Compression Therapy Used?
Compression therapy is widely recommended for conditions related to poor circulation and fluid retention. It is commonly used to treat:
- Chronic venous insufficiency (CVI): A condition where vein valves fail, causing blood to pool in the legs
- Edema: Swelling caused by excess fluid trapped in body tissues
- Deep vein thrombosis (DVT): A serious condition involving blood clots in deep veins
- Leg ulcers and chronic wounds: Particularly venous ulcers that require improved circulation
- Orthostatic hypotension: A drop in blood pressure when standing, often linked to poor circulation
In many cases, compression therapy in wound care can be profoundly beneficial for long-term recovery and prevention.
What Are the Benefits of Compression Therapy?
Managing Chronic Venous Insufficiency
Chronic venous insufficiency can lead to persistent swelling, discomfort, and open sores. Compression therapy supports proper blood flow, helping to:
- Reduce pressure in damaged veins
- Minimize swelling
- Lower the risk of complications such as varicose veins and ulcers
Improving Circulation
Sitting or standing for long periods can slow circulation in the lower limbs. Compression therapy helps maintain consistent blood flow, which is vital for tissue health and repair.
Reducing Swelling (Edema)
Fluid buildup in the legs and ankles can be painful and limit mobility. Compression encourages the body to reabsorb excess fluid, leading to noticeable relief and improved comfort.
Supporting Orthostatic Hypotension Management
By preventing blood from pooling in the lower extremities, compression therapy can reduce symptoms like dizziness and lightheadedness when standing.
Lowering the Risk of Blood Clots
Compression garments are often recommended for individuals at risk of clot formation, including travelers and post-surgical patients. By improving circulation, they help reduce the likelihood of DVT.
Enhancing Healing of Leg Ulcers and Chronic Wounds
One of the most important roles of compression therapy in wound care is its ability to accelerate healing. By improving oxygen and nutrient delivery to tissues, compression helps:
- Speed recovery
- Reduce discomfort
- Prevent recurrence of wounds
Beyond its primary medical uses, compression therapy may also provide:
- Reduced muscle fatigue and soreness
- Faster recovery after physical activity or surgery
- Improved flexibility and mobility
- Lower risk of infection due to better circulation
These added benefits make it a versatile option for both clinical treatment and ongoing maintenance.
Types of Compression Products
Different compression systems are used depending on the patient’s condition, mobility level, and treatment goals.
Bandages and Wraps
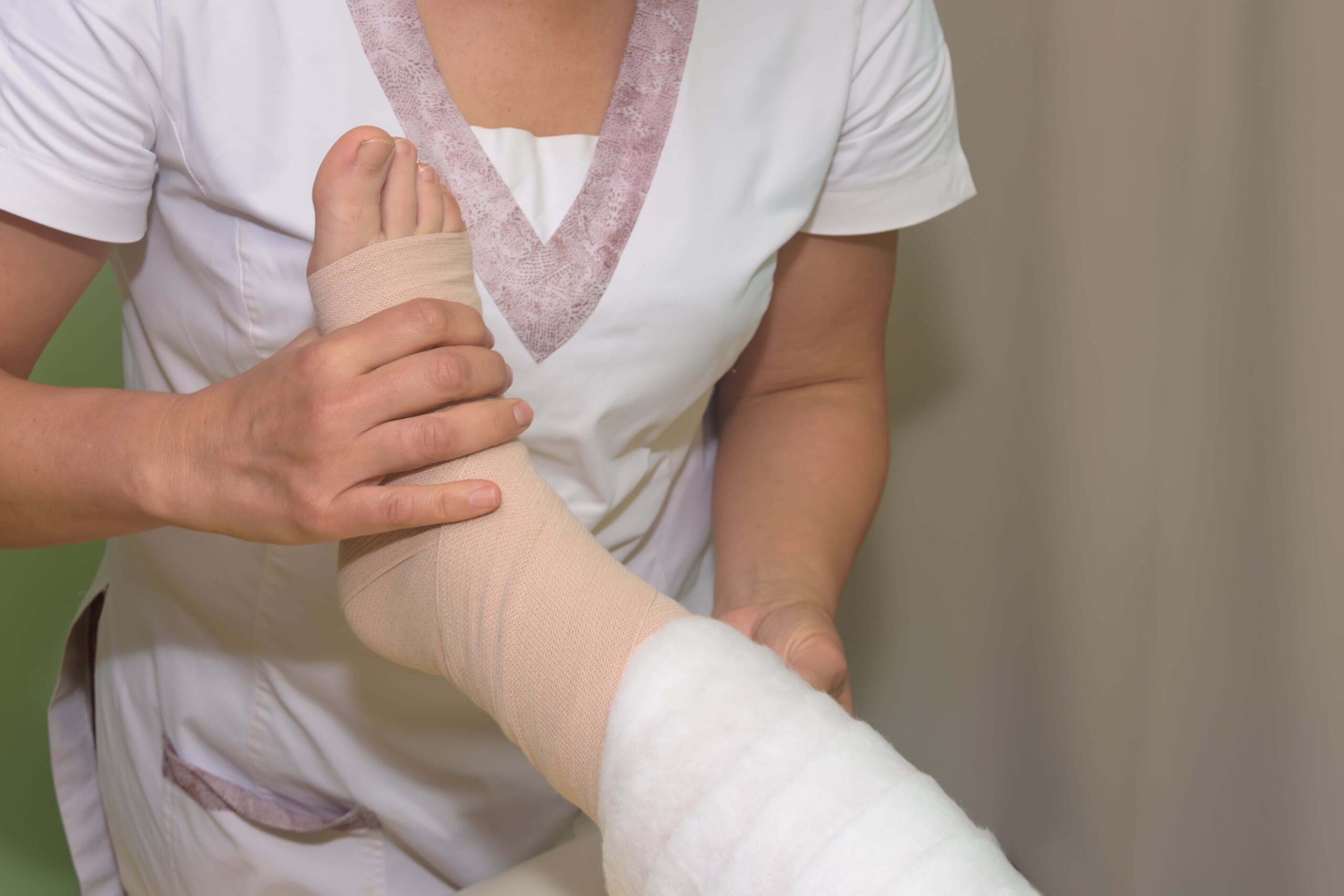
These include short-stretch, long-stretch, and multi-layer systems. They are often used in active wound treatment and must be applied correctly by a wound care specialist team to ensure proper pressure and effectiveness.
Compression Stockings and Socks
Typically used after wounds have healed, these garments help prevent recurrence. They are custom-fitted and available in varying pressure levels, extending to the knee or thigh.
Intermittent Pneumatic Compression (IPC)
This system uses a mechanical pump to inflate and deflate sleeves around the legs. While less common than bandages or stockings, it can be beneficial in specific cases requiring controlled, cyclic compression.
Is Compression Therapy Right for You?
Although highly effective, compression therapy is not suitable for everyone. Certain conditions require caution or alternative treatments, including:
- Peripheral arterial disease
- Severe heart failure
- Certain infections or skin conditions
A thorough evaluation is necessary before beginning treatment. A holistic wound care approach can provide real, lasting support. This considers the full picture of a patient’s health rather than focusing on a single symptom.
Professional Compression Therapy
Successful outcomes with compression therapy in wound care depend heavily on proper assessment, application, and follow-up. A trained provider will:
- Evaluate circulation and overall health
- Determine the appropriate level of compression
- Monitor progress and adjust treatment as needed
For patients who cannot easily travel, mobile wound care services provide access to expert treatment in the comfort of their home. This improves consistency and helps ensure that therapy is applied correctly over time.
Chronic wounds can significantly impact daily life, causing discomfort, limiting mobility, and increasing the risk of infection. Compression therapy addresses the underlying circulatory issues that often prevent wounds from healing.
FAQs About Compression Therapy in Wound Care
What is compression therapy in wound care used for?
Compression therapy in wound care is used to improve blood circulation, reduce swelling, and support the healing of chronic wounds, especially those caused by venous conditions such as leg ulcers and chronic venous insufficiency.
Are there different types of compression therapy?
Yes, compression therapy includes several options such as bandages, compression stockings, and intermittent pneumatic compression devices. The right type depends on the severity of the condition and the patient’s overall treatment plan.
Can compression therapy be done at home?
Yes, many patients receive treatment at home, especially with support from mobile wound care providers. However, proper guidance from a wound care specialist team is important to ensure safe and effective use.

