
We’re proud to provide comprehensive mobile wound care in Boston. Through a combination of in-clinic treatment and mobile visits, we support patients across the Greater Boston area with individualized plans designed to promote healing, reduce complications, and improve quality of life. Comprehensive Care When and How You Need It For many patients, visiting a specialized […]
Learn More
A scraped knee, a small cut from cooking, or a blister from new shoes may not seem like a big deal. Many minor injuries heal with basic first aid. However, when healing stalls or symptoms worsen, what looked simple can quickly become complicated. Knowing when to seek wound care can prevent infection, tissue damage, and […]
Learn More
Winter presents a unique set of challenges for skin integrity and wound healing, particularly for older adults and individuals managing chronic conditions. Through innovative wound care, we address both prevention and treatment, combining mobile wound care services with regionally located clinics to meet patients where they are while maintaining consistent clinical standards. At West Coast […]
Learn More
Navigating Medicare coverage can feel overwhelming, especially when ongoing treatment is required. At West Coast Wound & Skin Care, we can help patients make sense of how wound care services, supplies, and clinical decisions intersect with Medicare guidelines. Always, our goal is to reduce confusion, streamline access to treatment, and ensure care decisions are driven […]
Learn More
The 2026 CPT coding updates represent a meaningful shift in how wound care services are delivered, monitored, and reimbursed. At West Coast Wound & Skin Care, these updates support how we already provide comprehensive wound care. How 2026 CPT Updates Affect Wound Care Delivery The AMA’s 2026 CPT updates introduce hundreds of new codes reflecting […]
Learn More
Medicare Advantage (MA) is, all too often, not advantageous to those who need it. Members routinely face obstacles that slow down the wound care they desperately need. Prior authorization layers, repeated documentation requests, inconsistent coverage criteria, and long insurer review times can create delays that directly affect outcomes. These setbacks often halt procedures and therapies […]
Learn More
Insurance claim denials can disrupt treatment plans, cause unnecessary stress, and lead to delays in accessing the specialized wound care you or your loved one needs. Patients often assume that, once treatment begins, insurance approval is automatic. But insurers can deny claims for many reasons, even when the services are medically necessary. At West Coast […]
Learn More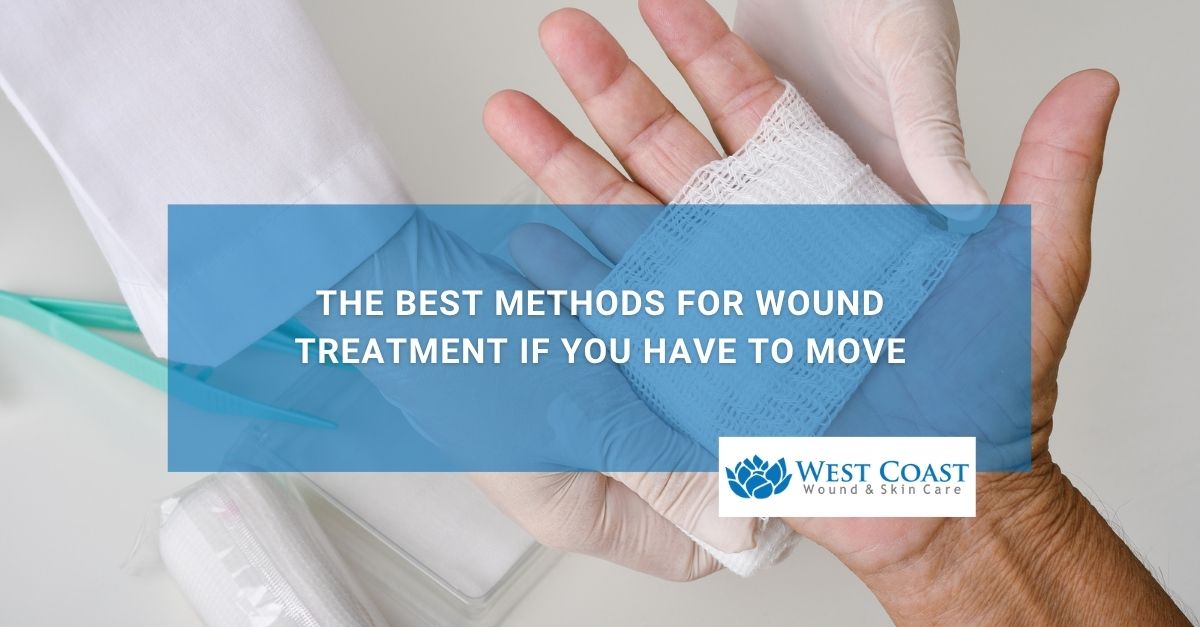
Often, rest is good for advanced wound treatment. However, you can’t stay motionless forever. Managing a serious or chronic wound requires a delicate balance between rest and daily life. Proper care often involves minimizing unnecessary movement to protect the delicate, regenerating tissues. Movement, while a natural part of life, can introduce stress, pressure, and friction […]
Learn More
The current 2025 government shutdown has introduced significant challenges across many sectors, with the healthcare industry feeling a considerable impact. For millions of Americans who rely on federal programs for their health needs, the shutdown caused instant concerns. At West Coast Wound Care, we will always provide high-quality advanced wound care to our patients. We continue to […]
Learn More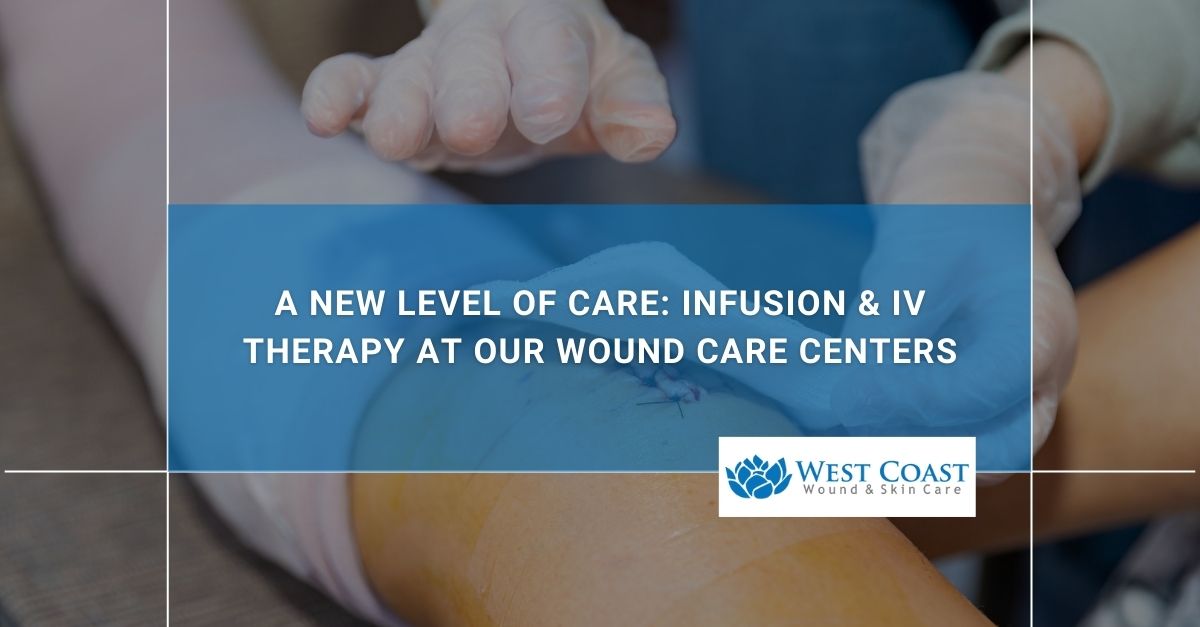
When wounds resist healing because of infection, poor circulation, or chronic disease, the right medical approach can make the difference between slow recovery and meaningful healing. At West Coast Wound & Skin Care, our advanced wound care centers offer advanced infusion and IV therapy as integral parts of our comprehensive treatment offerings. We bring together […]
Learn More