Arterial ulcers are a type of painful skin wound commonly found on the lower leg. These types of wounds generally don’t heal like other injuries because there is a lack of blood flow to the area; preventing much needed oxygen and nutrients from reaching the wound site. Even a small injury can develop into an ulcer without sufficient blood reaching it.
If left untreated, arterial ulcers can result in serious complications like infection, tissue necrosis, and in the worst-case scenario, amputation. Fortunately, with the help of wound specialists and proper wound care, arterial issues can be managed, treated, and in some cases even prevented.
What is an Arterial Ulcer?
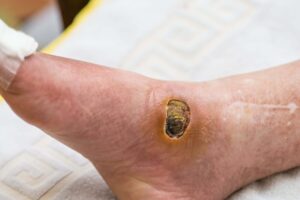 When an artery in your leg becomes blocked, poor blood circulation deprives leg tissue of oxygen and nutrients. As such, arterial ulcers are also often referred to as ischemic (restricted blood and oxygen flow) ulcers. If this continues, your skin and underlying tissue begin to die, creating an open wound – or an arterial ulcer (or arterial wound). This poor circulation also makes it difficult for red blood cells to carry the nutrients the wound needs, resulting in these types of wounds healing more slowly and increasing the risk of infection.
When an artery in your leg becomes blocked, poor blood circulation deprives leg tissue of oxygen and nutrients. As such, arterial ulcers are also often referred to as ischemic (restricted blood and oxygen flow) ulcers. If this continues, your skin and underlying tissue begin to die, creating an open wound – or an arterial ulcer (or arterial wound). This poor circulation also makes it difficult for red blood cells to carry the nutrients the wound needs, resulting in these types of wounds healing more slowly and increasing the risk of infection.
Causes of Arterial Ulcers
There are a number of reasons why arteries may be blocked resulting in arterial issues. Some of the most common causes of arterial blockage may include:
- High cholesterol
- Chronic kidney issues
- Atherosclerosis (arterial thickening) due to deposits of cholesterol and other lipids on vessel walls
- Smoking that weakens arterial walls
- Diabetes
- High Blood Pressure (Hypertension)
- Vasculitis
- Limited Mobility (sitting or lying in one position for too long)
- Restrictions to blood vessels due to peripheral vascular disease
- Trauma
- Increased age
Comorbidities like sickle cell anemia and rheumatoid arthritis also enhance the risk of an arterial ulcer. Moreover, foot deformities and poor footwear can also hamper blood circulation in the leg, leading to ischemic ulcers in areas where there is pressure from exercising, walking, or wearing footwear.
Signs and Characteristics of an Arterial Ulcer
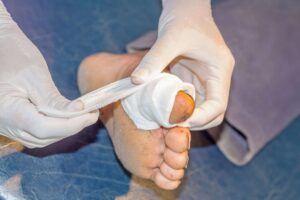 Arterial ulcers often occur on the toes, heals, or bony parts of the foot. They are typically characterized by a ‘punched out’ appearance, such that their round shape has well-defined margins, but the sore is deeper in the skin than the healthy tissue that surrounds it. The base of the wound can be yellow, brown, grey, or black in color. The wound itself can be quite painful, with discomfort typically worsening at night or at rest.
Arterial ulcers often occur on the toes, heals, or bony parts of the foot. They are typically characterized by a ‘punched out’ appearance, such that their round shape has well-defined margins, but the sore is deeper in the skin than the healthy tissue that surrounds it. The base of the wound can be yellow, brown, grey, or black in color. The wound itself can be quite painful, with discomfort typically worsening at night or at rest.
Its symmetrical shape and distinctive color can be accompanied by other signs such as:
- Deepness of the wound
- Coolness to touch, due to low blood circulation
- Reddening of the leg when it dangles and paleness when elevated
- Minimal hair growth on the limb with ulcers
- Dry, shiny, and thin skin and nails
- Tight skin
Unlike some other wounds, because low blood circulation is the primary cause of these types of ulcers they don’t bleed. The pulse in the affected area is also typically low and cool to the touch.
It’s common for affected patients to try to relieve pain by hanging their legs from the bed or sleeping in a chair. Additionally, you may experience cramping pains in the back of the legs and your glutes after exercise since your muscles are ill-equipped to meet the growing oxygen demands of the activity. In many cases, however, this pain will subside with rest.
Since the blood supply to this region is poor, white blood cells are in low supply. That means your body may have more difficulty warding off infections.
Some red flags to watch out for include fever (infection), discharge, numbness (nerve damage), and a foul odor. You should contact a wound care specialist or medical professional as soon as possible if you experience any of these symptoms; as delayed treatment can result in severe complications including amputation.
Arterial vs Venous Ulcers
Because arterial and venous ulcers both can occur on the lower extremities and share some characteristics, it can be difficult to tell them apart. That said, there are several key differences between both of these conditions such as:
- Location: Arterial ulcers typically affect the outer side of the ankle, feet, heels, or toes. Venous ulcers, on the other hand, typically appear below the knee or on the inner ankle.
- Causes: While arterial ulcers are often caused by damage to the arteries resulting from poor circulation, venous ulcers tend to be a result of damage to veins that impair blood flow to the heart and can be caused by conditions like varicose veins, blood clotting disorders, deep vein thrombosis, heart failure, obesity, and pregnancy.
- Appearance: Unlike arterial ulcers that appear punched out with distinct discoloration, venous ulcers can vary in how they look, have an irregular shape, be less deep, and have a more red appearance.
- Characteristics: Arterial ulcers are often painful and uncomfortable. Although venous ulcers can be associated with discomfort, itching, and swelling, at times they are painless unless infected. Additionally, unlike arterial ulcers, oedema and weeping are often associated with venous ulcers. Venous ulcers can also be associated with other symptoms than commonly found in arterial ulcers.
- Treatment: While surgery and other interventions are more common treatment approaches for arterial ulcers, compression therapy is the primary treatment for venous ulcers.
- It’s also important to note that it is possible to suffer from a combination of venous and arterial diseases. In such cases, your wound specialist will take into consideration both conditions when recommending treatment.
If you would like to learn more about Venous ulcers and how they are treated we highly recommend this in-depth guide we put together on the subject.
Treatment For an Arterial Ulcer
 Although in some cases, the body can heal arterial wounds on its own, as we discussed earlier, because of poor circulation to the area the process may be slower. While the above symptoms are common among arterial ulcers, it’s important to consult a wound specialist for a proper diagnosis and treatment. Your specialist will begin with a thorough assessment to determine the potential of healing and the best course of treatment.
Although in some cases, the body can heal arterial wounds on its own, as we discussed earlier, because of poor circulation to the area the process may be slower. While the above symptoms are common among arterial ulcers, it’s important to consult a wound specialist for a proper diagnosis and treatment. Your specialist will begin with a thorough assessment to determine the potential of healing and the best course of treatment.
There are a number of tests healthcare professionals can use that indicate vascular compromise, such as capillary refill time and a Beurger test (where the patient lies flat and raises their leg 45 degrees above horizontal for 1 minute). Visiting a wound care center also allows your specialist to address any underlying causes; a crucial aspect of treating arterial ulcers.
Diabetes, arterial disease, and kidney diseases are a few risk factors of arterial disease, which is why just treating the ulcer itself might not be sufficient for full recovery. Restoring blood circulation to the affected area is the primary goal of treatment for arterial ulcers along with treating underlying causes, preventing infection, removing pressure on the affected limb, and keeping the wound dry and clean with dressings.
Pressure on the sore can also be relieved through special shoes and orthopedic devices. The wound is kept dry and clean with bandages and dressings, which must be regularly changed.
While some dressings reduce discharge, others serve as an optimal medium for healing. Your specialist can recommend specific wound dressings based on the nature of your arterial wound.
Because infection can lead to rapid deterioration of an arterial ulcer, antibiotics may also be prescribed if there are any indications of an infection.
Most importantly, blood circulation must be re-established. In some cases, surgical options, such as angioplasty (balloon to open up the affected artery) and bypass (setting up a new pathway for blood flow), may be utilized.
Your specialist may also outline specific lifestyle changes such as exercising regularly, taking note of your sodium intake, quitting smoking, and managing your cholesterol, blood pressure, and blood sugar by switching to a healthier diet. Not only can these changes aid in the healing process but can play a role in preventing arterial ulcers from coming back.
Additional Tips for Managing Arterial Ulcers
Whether you are at risk of developing an arterial ulcer or are looking to reduce potential complications there are a few other steps you can take to help:
Taking Care of Your Feet and Legs
- Regularly examine your feet and legs for any indications of ulcers.
- Always protect your feet from injury and make sure your shoes fit properly.
- Avoid soaking your feet for extended periods of time.
- Avoid walking barefoot when possible.
Lifestyle Tips
- Avoid tobacco products that can harden the arteries.
- Regularly monitor and manage your blood pressure and cholesterol.
- Try not to be in one position too long and avoid sitting cross-legged.
- Stay hydrated and eat a healthy diet.
- Regularly exercising or walking if you’re doctor says it’s okay.
- Some patients find sleeping in a raised bed to be helpful as well.
Additionally, if you are recovering from an arterial ulcer at home your doctor may recommend:
- Regularly changing your dressing to keep the wound clean and dry.
- Trying to keep pressure off of your legs.
- Taking any prescribed medications as recommended.
- Wearing orthopedic shoes and/or compression wraps.
- Following additional recommendations on managing underlying conditions.
Specialized Healing For Arterial Ulcers and Chronic Wounds
Arterial ulcers sound scary, but recovery is possible with proper wound care and management. While your wound specialist focuses on treating the underlying disease and reestablishing circulation, there is much you can do as well. Keeping the wound dry by changing the dressing, taking your prescribed medicines, wearing orthopedic shoes, and adopting a healthy lifestyle can be an invaluable defense against arterial ulcers.
If you or someone you care for is suffering from an arterial ulcer or is at risk of developing one; the specialized team at West Coast Wound Center is here to help.
Through our fully integrated wound and dermatology care and high-quality services, we heal arterial ulcers 25% quicker than other practices.
Our specialized wound care staff is equipped with the expertise to treat a full range of wound types and skin concerns. Book an appointment at our wound care center today and discover how we can restore your quality of life.
