How do I know if my burn can be treated at home?
Small, first-degree burns that only affect the outer layer of skin can usually be managed at home. If the burn is large, deep, or located on sensitive areas like the face or hands, professional burn wound care is recommended.
Should I put ice on a burn?
No, ice can damage the skin and worsen the injury. Instead, run cool (not cold) water over the burn or use a damp compress to gently cool the area.
Types of Burns and Their Severity
Burns are categorized based on how deeply they affect the skin and underlying tissues:
- First-degree burns
- Affect only the outer skin layer (epidermis)
- Symptoms include redness, mild swelling, and pain
- No blistering (commonly seen with mild sunburns)
- Second-degree burns
- Extend into the dermis (second layer of skin)
- Often cause blisters, swelling, and significant discomfort
- Can be superficial or deep depending on tissue damage
- Third-degree burns
- Destroy all layers of the skin
- May appear white, charred, or leathery
- Nerve damage can reduce or eliminate pain sensation
- Fourth-degree burns
- Extend beyond the skin into muscle and bone
- Require emergency medical treatment
Some burns may include a combination of depths, which makes individualized burn wound care especially important.
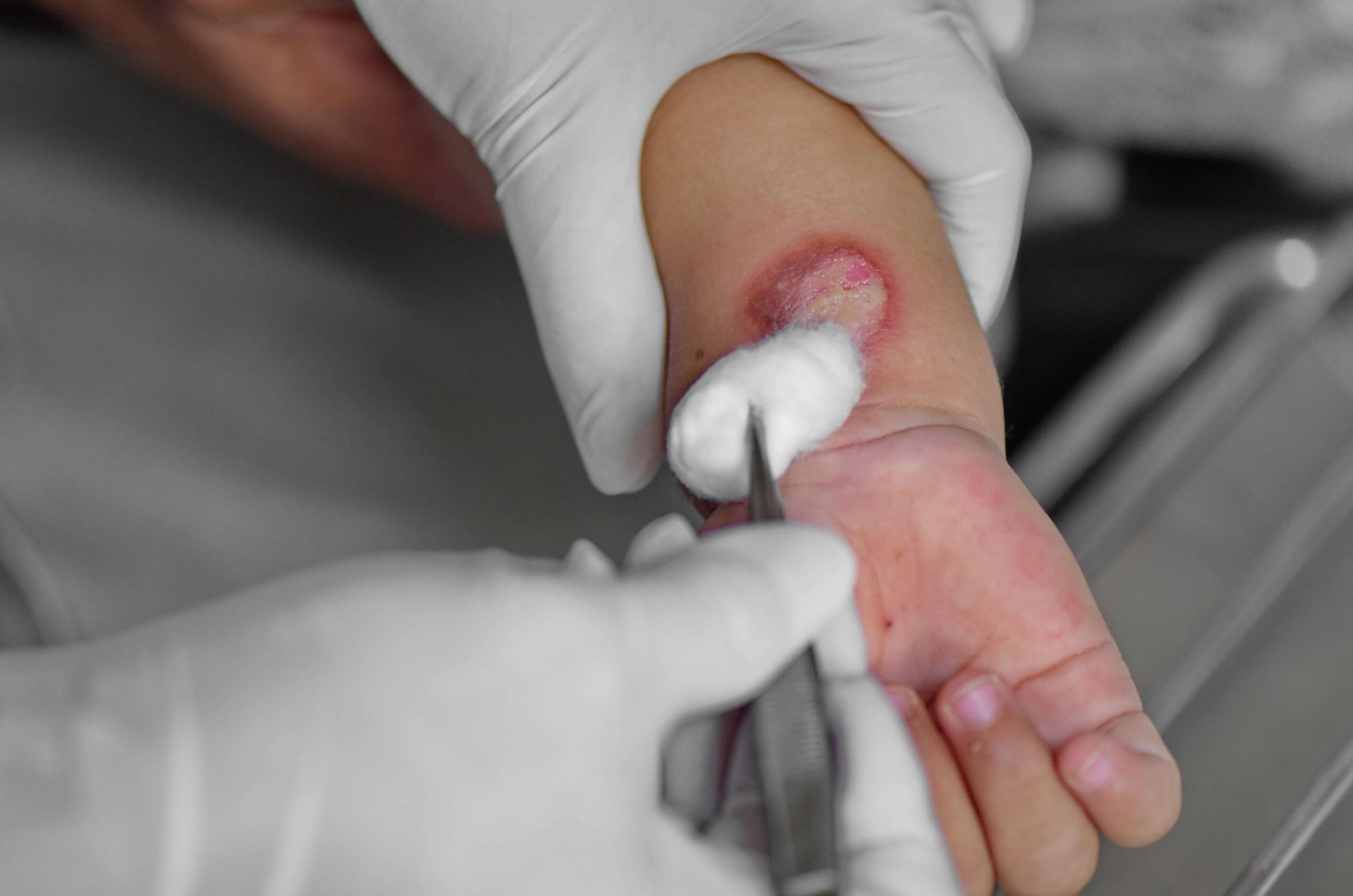
First-Degree Burn Wound Care at Home
Minor burns can often be treated safely at home if they are small and not located on sensitive areas such as the face, hands, feet, or genitals.
Steps to follow:
- Remove restrictive items
- Take off rings, watches, or tight clothing before swelling begins
- Cool the burn
- Run cool (not cold) water over the area for 10–15 minutes
- Avoid ice, as it can damage the skin further
- Apply moisture
- Use aloe vera or a gentle ointment to keep the skin hydrated
- This supports early stages of wound healing
- Protect with a dressing
- Cover the area loosely with sterile, non-stick gauze
- Keeps bacteria out while allowing airflow
- Manage pain
- Over-the-counter medications like ibuprofen or acetaminophen can help
- Check tetanus status
- Ensure vaccinations are current to reduce infection risk
If symptoms worsen or healing stalls, a wound care specialist team should evaluate the injury.
Treatment for Second- and Third-Degree Burns
Moderate to severe burns demand immediate and ongoing medical care. Proper burn wound care at this stage focuses on preventing complications and preserving as much healthy tissue as possible.
Initial first aid:
- Cover the burn with a clean, dry cloth
- Elevate the affected area to reduce swelling
- Watch for signs of shock (rapid pulse, shallow breathing, confusion)
Medical treatments may include:
- Antibiotic therapy
- Helps prevent or treat infections in deeper tissue
- Advanced dressings
- Non-adherent materials that maintain a clean, moist environment
- Fluid replacement
- IV fluids are often necessary to maintain hydration and circulation
- Pain control
- Prescription medications may be used for severe discomfort
- Debridement
- Removal of dead or damaged tissue to support healthy recovery
- Skin grafting
- Transplanting healthy skin to cover large or deep wounds
- Rehabilitation
- Physical therapy to restore mobility and minimize stiffness
These treatments are often part of a broader, holistic wound care approach that addresses both physical recovery and long-term function.
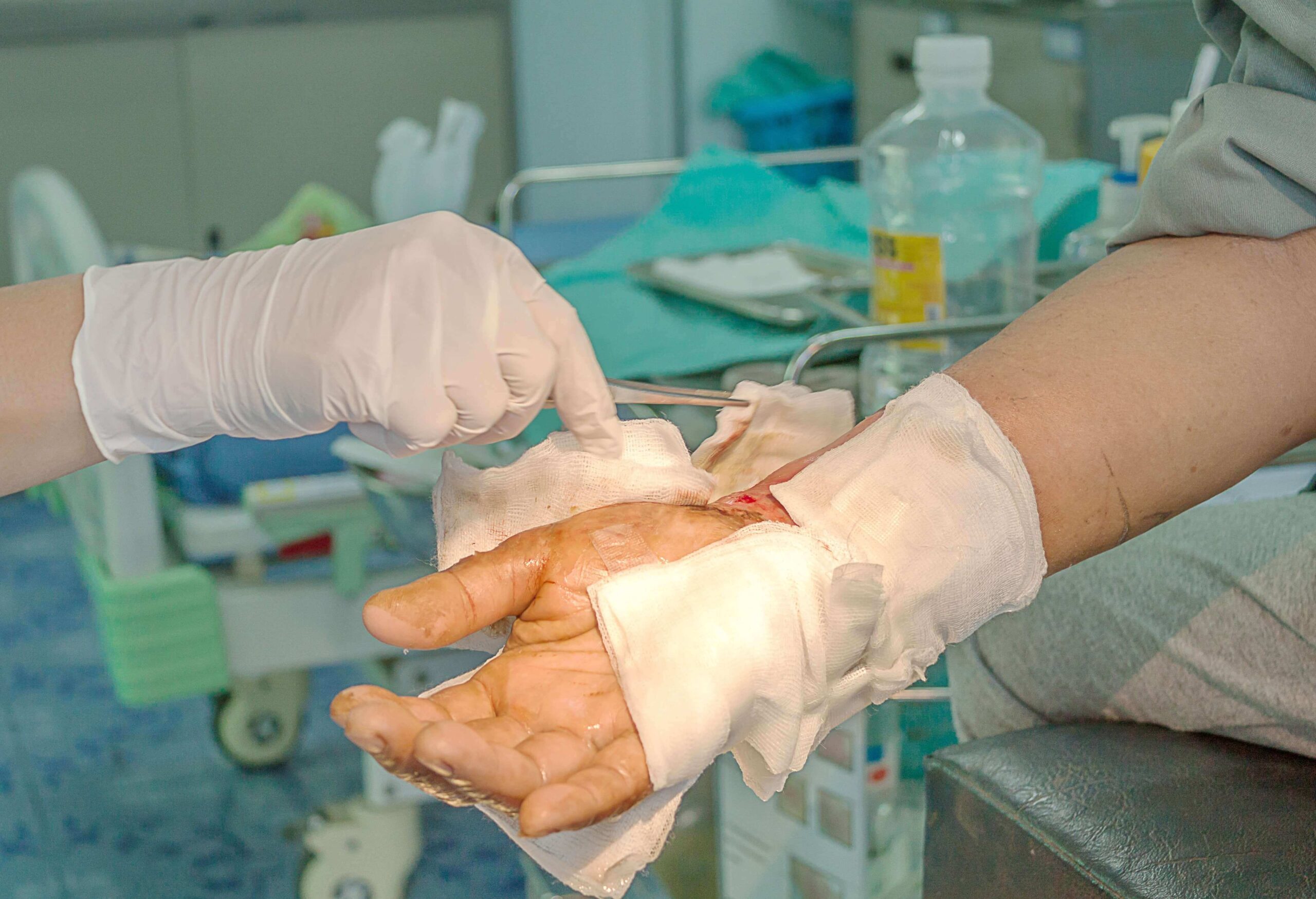
Managing Burn Blisters and Skin Tears
Blisters and fragile skin are common in burn injuries and must be handled carefully to avoid infection.
Blisters:
- Do not intentionally pop them
- If a blister breaks:
- Gently clean the area
- Apply a thin layer of ointment
- Cover with a sterile, non-stick dressing
Skin tears:
- Rinse the wound gently with clean water
- Apply light pressure to stop bleeding
- Use antibiotic ointment and cover with a protective dressing
Consistent burn wound care at this stage can significantly reduce scarring and complications.
Preventing Infection and Supporting Recovery
Infection is one of the biggest risks associated with burns. Maintaining a clean environment and monitoring symptoms closely are critical.
Watch for warning signs:
- Increased redness or swelling
- Pus or unusual discharge
- Fever or chills
- Worsening pain
Tips to promote healing:
- Keep the wound clean and properly dressed
- Avoid exposing the burn to direct sunlight
- Stay hydrated and maintain proper nutrition
- Follow all medical instructions carefully
For patients who cannot easily travel, mobile wound care services provide access to professional treatment at home, ensuring continuity and convenience.
When to Seek Professional Burn Wound Care
Not all burns should be treated at home. Medical evaluation is necessary if:
- The burn is larger than a few inches
- It involves the face, hands, feet, joints, or genitals
- The skin appears charred, white, or leathery
- There are signs of infection or delayed healing
- The injury was caused by chemicals or electricity
Specialized care ensures that every stage of burn wound care is handled properly, reducing long-term damage and improving outcomes.
FAQs About Burn Wound Care
Is it safe to pop burn blisters?
It’s best not to pop blisters, as they protect the underlying skin from infection. If a blister breaks on its own, clean it carefully, apply ointment, and cover it with a sterile dressing.
What are signs that a burn may be infected?
Watch for increased redness, swelling, warmth, pus, fever, or worsening pain. These symptoms may indicate infection and require prompt medical attention.
When should I see a specialist for a burn?
You should seek care if the burn is severe, not healing properly, or showing signs of infection. A medical provider can recommend advanced treatment options to support safe and effective recovery.
