Necrotic wound care plays a critical role in treating wounds that contain dead or damaged tissue. Without timely and effective intervention, these wounds can worsen quickly, leading to infection, delayed recovery, or serious complications.
What Are Necrotic Wounds?
Necrotic wounds form when tissue dies due to a lack of oxygen, poor circulation, infection, or trauma. This dead tissue not only slows recovery but also creates an environment where bacteria can thrive.
Common characteristics of necrotic wounds include:
- Eschar: Thick, dry, black or brown tissue that may feel leathery
- Slough: Soft, yellow or white fibrous tissue that can appear stringy
- Gangrene: Advanced tissue death, often accompanied by discoloration and odor
These wounds are frequently associated with underlying health issues such as diabetes, vascular disease, or prolonged immobility. Identifying necrosis early is a big part of effective necrotic wound care.
How can infection in necrotic wounds be managed?
Infections are treated with antibiotics, antimicrobial dressings, and proper wound cleaning. Close monitoring ensures that infections are controlled before they spread or worsen.
Can necrotic wounds be prevented?
Many necrotic wounds can be prevented with proper wound care, good nutrition, and management of chronic conditions. Regular skin checks and relieving pressure on vulnerable areas also help reduce risk.
Common Causes of Necrotic Wounds
Several conditions and events can lead to tissue death and wound necrosis. Recognizing these causes helps guide both treatment and prevention strategies.
- Infections: Untreated bacterial or fungal infections can destroy healthy tissue and lead to necrosis
- Vascular Disorders: Reduced blood flow from conditions like peripheral artery disease limits oxygen delivery to tissues
- Pressure Ulcers: Continuous pressure on certain areas of the body, especially in bedridden individuals, can restrict circulation
- Trauma: Burns, deep lacerations, and crush injuries may damage blood vessels and lead to tissue death
- Surgical Complications: Poor healing or post-operative infections can result in necrotic tissue formation
Each of these factors can significantly impact wound healing, making early intervention essential.
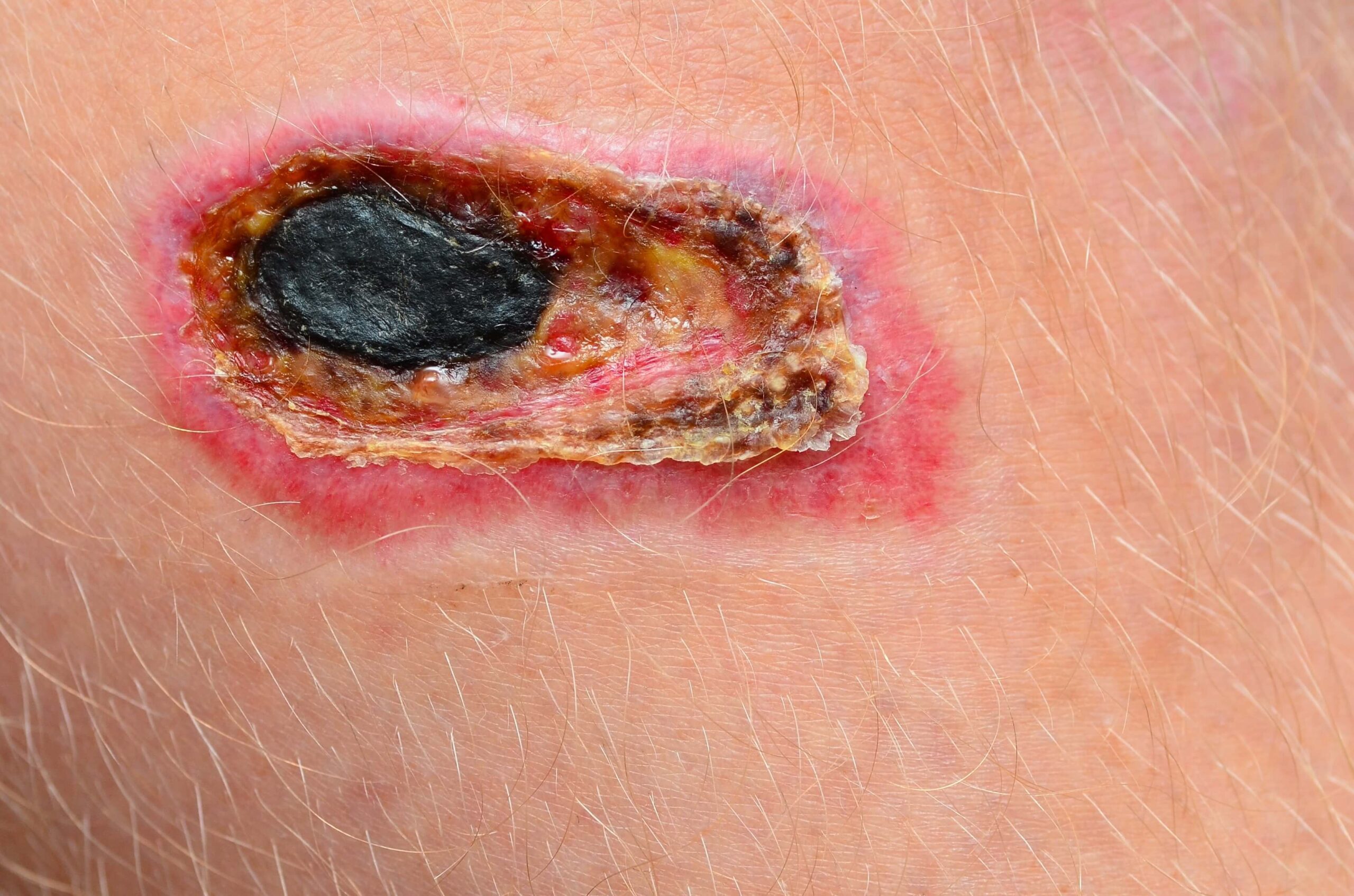
Steps in Necrotic Wound Care
Effective necrotic wound care requires a structured and personalized approach. Treatment plans are designed based on the severity of the wound, the patient’s overall health, and the underlying cause.
1. Thorough Assessment
A detailed evaluation is the first step. A wound care specialist team assesses:
- Wound size, depth, and location
- Presence of infection
- Circulation and tissue viability
- Patient health conditions that may affect healing
This assessment helps determine the most appropriate treatment path.
2. Debridement of Dead Tissue
Removing necrotic tissue is essential for recovery. Debridement allows healthy tissue to grow and reduces infection risk.
Common methods include:
- Surgical debridement: Rapid removal using medical instruments
- Mechanical debridement: Use of dressings or irrigation
- Enzymatic debridement: Topical agents that break down dead tissue
- Autolytic debridement: The body’s natural process supported by moisture-retentive dressings
- Biological debridement: Use of sterile larvae to remove dead tissue
The choice depends on the wound’s condition and the patient’s tolerance.
3. Infection Control
Necrotic wounds are highly susceptible to infection. Managing bacteria is a cornerstone of necrotic wound care.
Treatment may include:
- Topical or systemic antibiotics
- Antimicrobial dressings
- Regular wound cleaning and monitoring
Controlling infection not only protects surrounding tissue but also supports faster wound healing.
4. Moisture Balance
Maintaining the right level of moisture is essential. A properly balanced wound environment:
- Encourages tissue regeneration
- Prevents the wound from drying out
- Reduces the risk of further tissue damage
Dressings are selected to retain moisture while absorbing excess fluid.
5. Advanced Dressing Selection
Different wounds require different dressing types. Options include:
- Hydrogels: Ideal for dry wounds with necrotic tissue
- Foam dressings: Absorb excess exudate while protecting the wound
- Alginates: Suitable for heavily draining wounds
Choosing the right dressing is a part of holistic wound care, as it supports both comfort and recovery.
6. Nutrition and Hydration Support
Healing starts from within. Patients with necrotic wounds benefit from:
- High-protein diets to rebuild tissue
- Vitamins such as C and A for immune support
- Minerals like zinc to aid repair
- Proper hydration to maintain skin integrity
Without proper nutrition, even the best wound care strategies may fall short.
7. Pain Management
Necrotic wounds can be painful, especially during treatment. Managing discomfort improves the patient’s overall experience and compliance with care.
Pain relief strategies may include:
- Prescribed medications
- Topical anesthetics
- Gentle handling during dressing changes
8. Ongoing Monitoring
Regular follow-up is necessary to track progress and adjust treatment as needed. Wounds can change quickly, and consistent evaluation ensures optimal outcomes.
For patients who have difficulty traveling, mobile wound care services can bring professional treatment directly to their home, improving access and consistency of care.
Prevention Tips for Necrotic Wounds
Preventing necrotic wounds is often more manageable than treating them. Taking proactive steps can significantly reduce risk.
- Practice proper wound care: Clean and dress injuries promptly
- Relieve pressure regularly: Reposition frequently to avoid pressure ulcers
- Manage chronic conditions: Control diabetes and vascular disease
- Follow post-surgical instructions: Keep incisions clean and monitored
- Maintain a balanced diet: Support immune function and tissue repair
- Perform routine skin checks: Look for early signs of breakdown or discoloration
These strategies are especially important for individuals at higher risk, such as older adults or those with limited mobility.
Supporting Recovery With Comprehensive Care
Successful necrotic wound care often requires a combination of clinical expertise, patient education, and ongoing support. From initial assessment to advanced therapies, each step is designed to restore healthy tissue and prevent complications.
A coordinated approach that includes debridement, infection control, and personalized treatment planning can significantly improve outcomes. With the right care strategy in place, even complex wounds have a clear path toward recovery.
Necrotic Wound Care FAQs
What is necrotic wound care?
Necrotic wound care focuses on treating wounds that contain dead or damaged tissue. It involves removing non-viable tissue, preventing infection, and creating an environment that supports healing.
What causes a necrotic wound to develop?
Necrotic wounds can result from poor circulation, infections, pressure ulcers, trauma, or surgical complications. Underlying conditions like diabetes or vascular disease often increase the risk.
Why is debridement important in necrotic wound care?
Debridement removes dead tissue that can block healing and harbor bacteria. By clearing the wound, it allows healthy tissue to grow and reduces the risk of infection.

